Dr. Leeor Sommer who runs ENT hands-on workshops and Dr. Maria Ivankovic, lecturer extraordinaire on ENT emergencies discuss ENT Emergencies Pearls, Pitfalls, Tips & Tricks:
Dr. Ivankovic’s stepwise approach to managing epistaxis including the best local anesthetics, the use of ice to decrease nasal flow, who requires antibiotics, the management of hypertension in epistaxis, tranexamic acid for nose bleeds and managing posterior bleeds, tips for nasal and ear foreign body removal including the use of tissue adhesive, how to pick up and work up the dreaded Malignant Otitis Externa including key diagnostic pearls the best tests, sudden sensorineural hearing loss (‘The Bells’ Palsy of the Ear’) including how to save a patient from losing their hearing, Epiglottitis including diagnostic clues and imaging findings, Pharyngitis work-up and treatment: Do we need to work-up and treat with antibiotics at all? & The Toronto Throat Score, Tips and Tricks for peritonsillar abscess drainage, Hereditary and ACE-inhibitor associated Angioedema presentations and management including the use of C1 Esterase inhibitors.
Podcast: Play in new window | Download (Duration: 2:29:32 — 137.0MB)
Subscribe: Apple Podcasts
Written Summary and blog post by Claire Heslop, edited by Anton Helman November, 2013
Cite this podcast as: Sommer, L, Ivankovic, M, Helman, A. ENT Emergencies Pearls, Pitfalls, Tips and Tricks. Emergency Medicine Cases. November, 2013. https://emergencymedicinecases.com/ent-emergencies/. Accessed [date].
Epistaxis Management
Step 1: Visualize the bleed
Ensure proper orientation up-down orientation of nasal speculum (see image). If bleeding, ask pt to blow nose gently to clear clots.
Step 2: Anesthetize
Apply cotton pledget with 1:1 mix of oxymetazoline (Dristan or Afrin) & lidocaine, which may be more effective than cocaine (& less side effects), using bayonet forceps. Leave in place for 5–10 minutes with the nose *firmly* clamped.
Step 3: Cauterize
Remember eye and face protection, as silver nitrate causes sneezing. Cauterize dry edges of bleeding site (ie around the site, not on it), for 10–15 seconds maximum. Never cauterize both sides of the septum! Moisturize the area with petrolatum after cautery is complete.
Step 4: If bleeding continues, tamponize
Consider wrapping tampon on balloon-type in gelfoam or surgicel, which may encourage clotting in coagulopathic patients. Nasal balloons have greater patient satisfaction than tampons.
Management Pearls: Apply ice to the palate (popsicles, ice in the mouth) to reduce nasal blood flow up to 25%. Tranexamic acid 500 mg (1/2 vial of standard IV formulation or one 500mg tablet crushed) applied topically may also help anterior bleed [Zahed, 2013]. Can apply IV formulation, as a slurry with gelfoam.
Update 2021: A multi-center double-blind randomized study involving 496 patients with uncontrolled spontaneous epistaxis showed no benefit of adding topical TXA after simple first aid and topical vasoconstrictor are ineffective. Abstract
Who needs antibiotics for epistaxis?
No evidence supports Abx for immunocompetent patients with packing left in routine duration. However, if packing will be in place >72 hours, or patient is immunocompromized, add either amox/clav or cefuroxime. Packing should be left in at least 48–72 hours, or longer if patient is supra-therapeutic on anticoagulants. Have patients follow up in the ED on third day for packing removal.
Does elevated blood pressure cause epistaxis?
There is no evidence that hypertension causes nosebleeds. Usually high BP results from pain or anxiety. Our experts recommend treating these symptoms to manage hypertension in epistaxis patients.
Posterior Epistaxis
More rare, but can have more serious consequences. Suspect posterior bleeds in elderly patients, patients with brisk bleeds that cannot be directly visualized, or patients who have ongoing bleeding despite bilateral anterior packing. These patients require aggressive treatment in a monitored setting (if bleeding is severe, packing procedures may trigger vagal response), IV access, fluids, and ENT consultation for admission and IV antibiotics. Packing requires both anterior and posterior packing, usually by double packing balloons. Avoid overinflating, and secure anterior packs centrally to avoid alar necrosis.
Nasal Foreign Bodies
Tips for nasal foreign body
- First try positive pressure; either “parent’s kiss” [Koppuravuri, 2010], or puff from bagvalve mask over the mouth, with the opposite nare occluded – see video
- To reduce nasal swelling, apply a 1:1 mix of oxymetazoline (Dristan or Afrin) & lidocaine
Ear Foreign Bodies
Tips for ear foreign body
- Pull posteriorly on the pinna, or use a pediatric nasal speculum to see
- Try irrigation to remove small, nonwedged objects which aren’t likely to expand when wet
- Use 2% lidocaine to kill insects before removal, and for analgesia
Recommended tools: A right angle L-hook is ideal for beads and round objects, as is a suction-tipped catheter. A cerumen removal loop, or alligator forceps may also be used.
Tissue adhesive applied to the wooden end of a cotton swab stick may be used for objects that are difficult to grasp, but avoid adhering to ear canal (3). Apply glue and hold for 20–30 seconds, then extract.
After removal always check for more objects, in both nostrils and both ears!
REFER ASAP ALL BUTTON BATTERIES and MAGNETS! Chronic, impacted, or penetrating foreign bodies, and objects that may swell (beans, corn) should be seen urgently (12–24h). Round, tightly wedged objects should be referred, as ENT may have better success. Prescribe Ciprodex if ear canal has been damaged.
For excellent videos on basic ENT procedures see Short Sharp Scratch Videos
Malignant Otitis Externa
Suspect malignant otitis externa in patients with diabetes and ear pain. This aggressive, rare type of otitis externa can progress to meningitis, encephalitis, brain abscess, and cavernous venous thrombosis. The challenge is to catch it early, when treatment will be most successful.
Key Diagnostic Clues in Malignant Otitis Externa
Most cases occur in diabetics, or the immune suppressed. Be suspicious of pain out of proportion, or ear pain with trismus or jaw pain. Check for cranial nerve findings (typically facial nerve CNVII, but also CNIX, X and XI, if jugular foramen involved). Inspect auditory canal carefully for white-pink granulation tissue where cartilage and bone meet. If pre-test probability is low, order ESR. If ESR is high, or pre-test probability is high, refer these patients to ENT!
Imaging Options for Malignant Otitis Externa
CT scanning may show temporal bone calcium loss and osteitis (not sensitive!, looks for alternate diagnoses). The most sensitive test is a bone scan, looking for osteoclast and osteoblast activity.
Treatment of Malignant Otitis Externa
Typically oral cipro for 6–8 weeks, with surgery considered in select severe cases. Always swab and culture any discharge from the ear before starting treatment. 95% are caused by pseudomonas. All unwell patients should be admitted. Even well-appearing patients should only go home if they will be seen by ENT within 12–24 hours, and going home with supervision and instructions.
Sudden Sensorineural Hearing Loss
Sudden sensorineural hearing loss: “The Bells’ Palsy of the Ear” is a diagnosis of exclusion in which unilateral hearing loss occurs over hours, or overnight. Patients may present with vertigo, and at least 1/3 will have permanent hearing loss. Carefully examine cranial nerves, and elicit history of trauma, infection, or pain, and look for signs of infection, or ear canal obstruction. Also be suspicious for a posterior circulation stroke, which may also present as hearing loss!
Hum test to assess type of hearing loss
Ask patient to hum, and then tell you which ear hears loudest. Humming is louder in affected ear in conductive hearing loss, and louder in unaffected ear in sensorineural hearing loss.
Refer these patients to ENT for imaging and audiometric testing. Start steroids (1mg/kg prednisone for 10 days) and antivirals (famcyclovir 500mg tid, or valcyclovir 1g tid for 1 week). For patients with po steroid contraindications, tympanic steroid injections by ENT may help.
Epiglottitis
In patients with fever & sore throat and a normal appearing pharynx, think epiglottitis! Stridor and tripoding are clues for impending obstruction which can occur suddenly. These are predicted difficult airways! Involve ENT and anesthesia early. Intubate in the OR, with a surgical airway prepared!
Do an X-ray for epiglottitis?
Our experts recommend visualization by fiberoptic nasal pharyngoscopy.
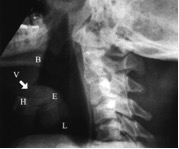
If an X-ray is done, look for the “thumbprint sign” (E), tissue swelling around hyoid bone (H). Look for the ‘vallecula’ sign (arrow, V), at the tongue base (B), which is positive if no air pocket extends toward hyoid bone [Lewis, 2013].
Update 2017: A retrospective review comparing ED physician and radiologist assessment of acute epiglottitis on neck radiography showed an epiglottis width of >6.3 mm had the best diagnostic accuracy, with good inter-observer agreement. The false-negative diagnosis rate was 31.9% and previous oral antibiotic usage was an independent risk factor of false negative results. Abstract
Antibiotics: IV ceftriaxone or cefotaxime, plus vanco if septic. Most common pathogen is H. influenza, but numerous other bacteria, viruses, and airway injuries have been implicated.
Should we give antibiotics for Pharyngitis?
Only ~10% of pharyngitis cases are caused by strep, and there is little (if any) evidence that treating strep throat prevents glomerulonephritis, peritonsillar abscess or rheumatic fever in North America. Abx shorten length of illness by only 16hrs! CDC recommends antibiotics only if Centor score is 4 (1 point for fever, tonsilar exudate, no cough, tender anterior lymph nodes). IDSA guidelines support Abx only if rapid swab or culture are positive. Our experts recommend the Toronto Throat Score, a modified Centor score which adds 1 point for 3–14 year olds, and subtracts 1 point from >45 year old patients [McIsaac, 2004].
TTS Score 0–1: no swab, no Abx.
TTS Score 2–3: swab for rapid strep test, treat based on results,
TTS Score 4: antibiotics, no testing.
Oral penicillin is antibiotic of choice. Use macrolide if allergic, or 1st gen cephalosporin if reaction is not anaphylactic. NSAIDs, Tylenol and lozenges help symptom relief. Not enough evidence supports steroid use.
See RebelEM’s review of the literature for antibiotics in acute pharyngitis here.
Update 2017: Single, oral low-dose steroids (dexamethasone 10mg or 0.6mg/kg) were two times more likely to provide complete pain relief at 24 hours in patients with sore throats of any cause, with no increase in serious adverse side effects. Abstract
Who gets testing for mono?
Our experts recommend mono test if history is suggestive, or for pregnant women. However, the test has higher false-negative rate early in disease course (sens 85%, spec >99%).
Update 2017: A recent systematic review of 105 studies has found that rapid strep testing has an overall sensitivity of 86.2% and a specificity 93.7%. This suggests it is a reasonably accurate diagnostic test for acute streptococcal pharyngitis. Abstract
Peritonsillar Abscess: When to suspect it & How to drain it
Suspect PTA with sore throat, “hot potato voice”, trismus, and asymmetric tonsils with uvula deviation. Point of care ultrasound may be as sensitive as CT scanning (up to 90%).
Drainage tips
- Use needle and scalpel with plastic guard trimmed to keep penetration ≤1cm. Use headlamp with tongue depressor, or light source, i.e. video laryngoscope. Prepare suction.
- Anesthetize with lidocaine spray, and inject 2% lido+epi into fluctuant area. Wait a few minutes, then make approx. 1cm incision into anterior/ medial tonsil over fluctuant spot.
- Use blunt dissection with hemostat inferiorly and laterally to locate abscess. Suction while gently expressing pus.
Angioedema
Hereditary and acquired angioedema from ACE inhibitors causes localized or diffuse soft tissue swelling, airway compromise and death. Take a family, allergy, and med history. Some patients present with isolated severe ABDO PAIN +/- free fluid on imaging. ACEi angioedema can occur years after the pt took ACEi. Examine the airway carefully! Look for stridor, swelling, hoarseness, and voice changes, which predict need for definitive airway [Ishoo, 1999]. If suspicious of laryngeal edema, visualize by fiberoptic nasopharyngoscopy.
Involve ENT and anesthesia early, with surgical airway ready, as attempt to intubate may increase swelling.
Treat using IM epinephrine (0.3-0.5 mg IM); also consider nebulized epi. For hereditary angioedema, treat with concentrated CI esterase inhibitors (Berinert and Cynrize in Canada), or 2–4 units of fresh frozen plasma. Neither ACEi nor hereditary angioedema patients benefit from steroids or H1 and H2 blockers. Once symptoms improve, most patients may be observed for 4–6 hours, then sent home, with good follow-up and an EpiPen [Wilkerson, 2012].
Dr. Helman, Dr. Sommer and Dr. Ivankovic have no conflicts of interest to declare.
References
Epistaxis:
Zahed, R et al. Am J Emerg Med. 2013;31:1389. www.ncbi.nlm.nih.gov/pubmed/23911102
Foreign Bodies:
Koppuravuri, MR. Emerg Med J. 2010;27:480. www.ncbi.nlm.nih.gov/pubmed/20562151
Pharyngitis:
McIsaac, WJ et al. JAMA. 2004;291:1587. www.ncbi.nlm.nih.gov/pubmed/15069046
Angioedema:
Ishoo, E et al. Otolaryngol Head Neck Surg. 1999;121:263. www.ncbi.nlm.nih.gov/pubmed/10471868
Wilkerson W. Emerg Med Pract. 2012;12:11. www.ncbi.nlm.nih.gov/pubmed/23137438
Lewis, LM. J Emerg Med. 2013;S0736. www.ncbi.nlm.nih.gov/pubmed/23992848
Now test your knowledge with a quiz.





For pharyngitis, see this amazing runthrough from BroomDocs, Casey Parker: https://broomedocs.com/2014/09/on-sick-kids-sore-throats-swabs-and-such/
Thanks for the post!
Peter
http://www.akutmedicineren.dk