In part 2 of our round-table discussion on EM Cases with sports medicine guru Dr. Ivy Cheng and orthopedic surgeon Dr. Hossein Mehdian we elucidate some key commonly missed uncommon orthopedic injuries that if mismanaged, carry significant long term morbidity. Injuries of the tendons and ligaments are often overlooked by emergency providers as relatively benign injuries and generally are not well understood.
Syndesmosis Injuries typically occur in impact sports. They are missed in about 20% of cases, as x-rays findings are often subtle or absent. The mechanism, physical exam findings, such as the Hopkin’s Test, and associated injuries are important to understand to help make the diagnosis and provide appropriate ED care.
Distal Biceps Tendon Rupture is almost exclusively a male injury and occurs in a younger age group compared to the Proximal Biceps Rupture. It is important to distinguish these injuries as their management and outcomes are different. The mechanism and physical exam findings of Distal Biceps Tendon Rupture, such as the Hook Test, are key in this respect.
Quadriceps Tendon Rupture is often misdiagnosed as a simple ‘knee sprain’, but should be consideration for surgical intervention. Quadriceps tendon ruptures are more commonly seen in patients older than 40 years and are more common than patella tendon ruptures which are more commonly seen in patients under 40 years of age. Interestingly, up to 1/3 of patients present with bilateral quadriceps tendon ruptures, so comparing to the contralateral knee may be misleading. There is a spectrum of knee extensor injuries that should be understood in order to provide proper care, with the Straight-Leg-Raise Test being abnormal in all of them. This is of the most important physical exam maneuvers to perform on every ED patient with a knee injury. The x-ray findings of these injuries may be subtle or absent, and proper immobilization of these injuries is important to prevent recoil of the tendon.
Patients with calf pain and Gastrocnemius Tears are often misdiagnosed as having a DVT. In fact, one small study showed that gastrocnemius tears were misattributed to DVT in 29% of patients. This confusion occurs because sometimes patients who suffer a gastrocnemius tear report a prodrome of calf tightness several days before the injury, suggesting a potential chronic predisposition. With a good history and physical, and POCUS if you’re skilled at it, needless work-ups for DVT can be avoided.
For well thought out approaches, pearls and pitfalls, to these 4 Commonly Missed Uncommon Orthopedic Injuries, listen to the podcast and read the rest of this blog post….
Podcast: Play in new window | Download (Duration: 46:26 — 42.6MB)
Subscribe: Apple Podcasts
Written Summary and blog post prepared by Keerat Grewal, Edited by Anton Helman, Jan 2015
Cite this podcast as: Mehdian, H, Cheng, I, Helman, A. Tendons and Ligaments – Commonly Missed Uncommon Orthopedic Injuries Part 2. Emergency Medicine Cases. January, 2015. https://emergencymedicinecases.com/episode-58-tendons-ligaments-missed-orthopedic-injuries/. Accessed [date].
Go to part 1 of this 2-part podcast on commonly missed uncommon orthopedic injuries
Click on the EM Cases Summary Card for each individual chapter
Syndesmosis Orthopedic Injuries
Syndesmosis injuries typically occur in impact sports. They are missed in about 20% of cases, as x-rays findings are often subtle or absent.
Question: What is the mechanism of a syndesmosis injury?
Syndesmosis injuries, or ‘high ankle sprains’ typically result from a rotational force, whereby external rotation of the ankle +/- hyperdorsiflexion overstretch the sydesmosis that lies between the distal tibia and fibula. This mechanism of injury is far less common than the classic ankle sprain as a result of an inversion mechanism.
Question: What are the 3 common physical exam findings of a syndesmosis injury?
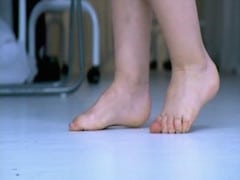
- Toe walking: Inspect the patient’s gait: patients may not weight bear appropriately, and may walk on their toes to prevent painful dorsiflexion.
Patients may have anterior ankle swelling and pain with palpation at the syndesmosis.
In a syndesmosis injury, ensure there is no concomitant deltoid ligament injury, which would result in an unstable ankle injury. Therefore, examine the medial aspect of the ankle for pain and stability.
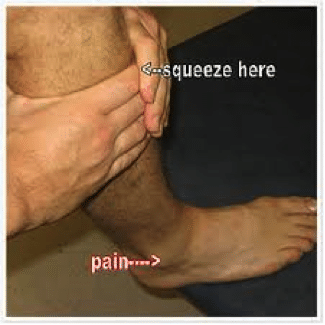
- Perform the Squeeze/Hopkin’s Test (see Fig 2): the tibia and fibula are squeezed together at the mid-calf level. This will result in pain at the syndesmosis, which is at the base of the tibia/fibular junction, near the talus.
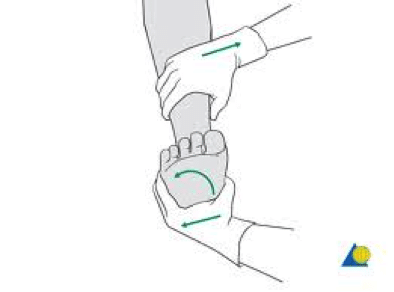
Try to reproduce the injury with an External Rotation Test (see Fig 3): the patient’s leg should be stabilized with the hip and knee flexed to 90 degrees. Holding the patient’s foot and externally rotating it with a small amount of dorsiflexion, will llicit pain at the syndesmosis.
Question: What are x-ray findings of a syndesmosis injury?
There are three common x-ray findings:
1.
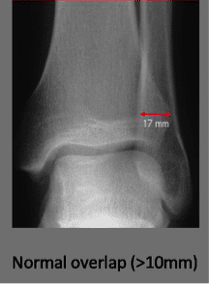
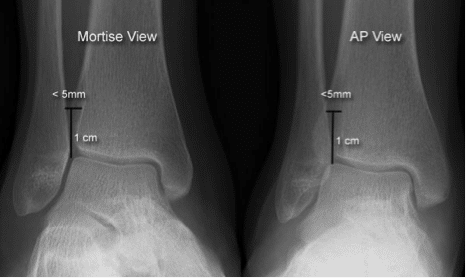
- Decreased tibio-fibular overlap:
- normally > 6mm of overlap on the AP view and > 1mm on mortise view
2.
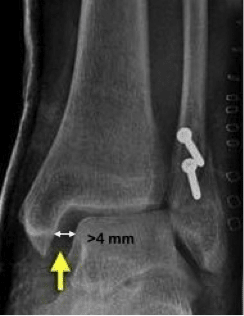
- Increased medial clear space
- normally ≤ 4 mm
3.
- Increased tibiofibular (syndesmosis) clear space
- normally < 5mm on AP and mortise views
Question: What is the appropriate ED management for a patient with a suspected syndesmosis injury who has normal x-rays?
Patients should be non-weight bearing in a walking boot or back slab. These patients should be followed up by orthopedics.
However, if you suspect widening of the syndesmosis, the joint may be subluxed, and the patient may need screw fixation. An orthopedic consultation would be prudent.
Question: While syndesmosis injuries may occur in isolation, they are often associated with other injuries. What other injuries are commonly associated with syndesmosis injuries?
Ankle fractures (Weber B and C), base of 5th metatarsal fracture, proximal fibula fracture.
Distal Biceps Tendon Rupture in Orthopedic Injuries
Distal Biceps Tendon Rupture is almost exclusively a male injury and occurs in a younger age group compared to the proximal biceps rupture. It is important to distinguish these injuries as their management and outcomes are different.
Question: What are the mechanisms of injury in a biceps tendon rupture?
Proximal biceps tendon ruptures typically occur in older patients with age-related degeneration of the tendon and who often have rotator cuff symptomology. There is usually no obvious mechanism.
Distal biceps tendon ruptures typically occur in younger patients, such as construction workers or weight lifters with chronic repetitive microtrauma that causes weakening of the tendon that attaches to a well-built muscle. This large bicep muscle is capable of a sudden massive eccentric contraction that tears the tendon. This occurs almost exclusively in males.
Question: What are the physical exam findings of biceps tendon ruptures?
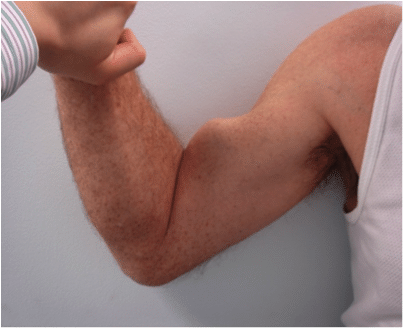
In both distal and proximal biceps tendon ruptures, a ‘Popeye’ sign (named after the old cartoon ‘Popeye The Sailor Man’ is typical.
In a distal biceps tendon rupture, you will often see ecchymosis on the anterior aspect of the elbow. There is usually decreased force of supination and/or pain with supination.
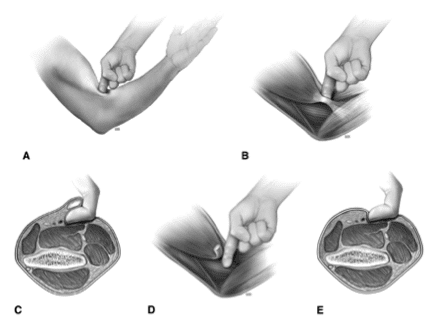
Look for the Hook Sign: use your index finger and go lateral to the insertion of the biceps and hook your finger around the biceps tendon. If there is no Hook Sign (an empty space) – there is likely a distal biceps rupture.
Question: How does the management of distal biceps tendon rupture differ from that of a proximal biceps tendon rupture?
Patients with a distal biceps tendon rupture should be immobilized, with early referral to orthopedics, as surgical repair within 2 weeks is desirable to avoid tendon retraction.
Quadriceps Tendon Rupture and The Spectrum of Quadriceps Mechanism Dysfunction
Quadriceps tendon rupture is often misdiagnosed as a simple ‘knee sprain’, and is not given appropriate, immediate follow-up for consideration of surgical intervention. Quadriceps tendon ruptures are more commonly seen in patients older than 40 years and are more common than patella tendon ruptures which are more commonly seen in patients under 40 years of age. Interestingly, up to 1/3 of patients present with bilateral quadriceps tendon ruptures, so comparing to the contralateral knee may be misleading.
Question: What is the spectrum of injuries in quadriceps mechanism dysfunction and how can you differentiate between them?
The spectrum of injuries includes: quadriceps tendon rupture, patellar fracture, and patellar tendon rupture.
All three injuries present with an inability to straight leg raise, with pain and an effusion around the knee. In older patient, those with diabetes and patients who have recently been on Ciprofloxacin, the injury is usually minimal, and you should be suspicious of quadriceps tendon rupture. In younger patients with significant injury, be suspicious of patellar tendon ruptures. With direct injury to the knee (i.e. fall or MVC) consider a patellar fracture.
Question: What are physical exam findings in quadriceps mechanism injuries?
All three injuries present with an inability to perform a straight leg raise.
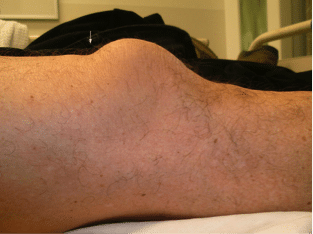
In a quadriceps tendon rupture, you can usually palpate a gap in the tendon above the knee. You may be able to see a suprapatellar gap when inspecting the knee from the side.
The triad of acute knee pain, inability to actively extend the knee and a suprapatellar gap clinch the diagnosis of quadriceps tendon rupture.
In a patellar fracture, patients will have tenderness over the patella. In a patellar tendon rupture, there will be a gap distally in the tendon below the patella.
Question: What are the typical x-ray findings in quadriceps tendon injuries?
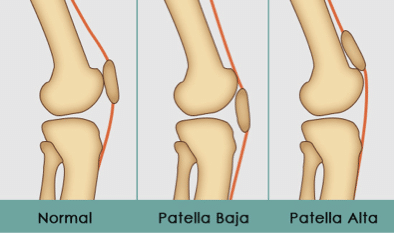
Usually patients have normal x-rays. With a quadriceps tendon rupture, you may see patella Baja (patella rides lower than usual). In a patellar tendon rupture, you may see patella Alta (patella rides higher than usual).
Question: What is the ED management of patients with a suspected quadriceps tendon rupture?
These patients require a knee immobilizer (e.g a Zimmer Splint). These patients can be weight bearing, and should have orthopedics follow up within a few days for surgical consideration.
Clinical pitfall: Quadraceps mechanism injury is one of the only injuries that requires a knee immobilizer. Meniscal tears, ACL, MCL and PCL injruries are often inappropriately immobilized in a Zimmer splint.
Gastrocnemius Tears in Orthopedic Injuries
Patients with calf pain and Gastrocnemius tears are often misdiagnosed as having a DVT. In fact, one small study showed that gastrocnemius tears were misattributed to DVT in 29% of patients. This confusion occurs because sometimes patients who suffer a gastrocnemius tear report a prodrome of calf tightness several days before the injury, suggesting a potential chronic predisposition. With a good history and physical, and POCUS if you’re skilled at it, needless work-ups for DVT can be avoided.
Question: What is the mechanism of injury in a gastrocneumius tear?
This injury typically occurs in sports requiring jumping or running up a hill, when a forceful push-off with the foot causes the gastrocnemius to attempt a forceful contraction against an already lengthened state. The gastrocnemius tear injury is also known as ‘Tennis Leg’ or the ‘Weekend Warrior’ because it usually occurs in people who are intermittently active in sport.
Question: How can a gastrocneumius tear be differentiated from a DVT?
In DVT, the affected leg may be more swollen then the other leg – this is not usually seen in a gastrocnemius tear. If there is swelling in a gastrocnemius tear, it is usually isolated to the medial aspect of the leg.
You may be able to palpate a divot between the junction of the gastrocnemius muscle and tendon in the setting of a complete tear. And finally, you may see early bruising.
Question: What are key physical exam findings in a gastrocnemius tear?
Patients will have tenderness of the entire medial gastrocnemius muscle, but will be more painful at the medial musculotendinous junction. You may be able to see a visible defect in the medial aspect of the gastrocnemius or palpate a gap in the muscle.
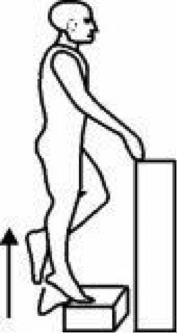
Perform a Calf Raise Test, where the patient in a standing position plantarflexes one ankle so that they stand up on their tip-toes with one leg. In an Achilles tendon rupture, patients will not be able to perform this test. In a gastrocnemius tear, this test will reproduce the pain, but patients can partially complete the test.
Question: What is the role of imaging for a gastrocnemius tear?
X-rays have no value. A non-urgent ultrasound, while it has not been studied in any large RCTs, can be considered as an outpatient, or a POCUS, if you have the necessary skills. It is important in your request for an ultrasound, to ask the radiologist to look for a gastrocnemius tear in particular.
Question: What is the ED management for patients with a gastrocnemius tear?
Conservative management with ‘RICE’ (Rest, Ice Compression & Elevation) and early weight bearing as tolerated is the treatment of choice. Early physiotherapy is important, as well as explaining to the sportsperson that it may take 3-4 months before they are back to full participation.
Consider an ankle stirrup or brace in a position of maximal tolerable dorsiflexion for patients who are experiencing severe pain with minimal ankle ROM, as studies have shown an increased rate of healing with ankle bracing.
Part 1 on Commonly Missed Uncommon Orthopedic Injuries including Lisfranc and Perilunate injuries here
For more on missed orthopedic injuries on EM Cases:
Episode 1 Occult Fractures and Dislocations
Episode 52: Commonly Missed Uncommon Orthopedic Injuries
Key References
- Heest, TJ & Lafferty, PM. Injuries to the ankle syndesmosis. 2014. J Bone Joint Surg Am, 96(7): 603-13. Abstract
- Lin, CF, Gross, ML, & Weinhold, P. Ankle syndesmosis injuries: Anatomy, biomechanics, mechanism of injury, and clinical guidelines for diagnosis and intervention. 2006. J Orthop Sports Phys Ther, 36(6): 372-84. Abstract
- Yilmaz, C, Orgenc, Y, Ergenc, R, & Erkan, N. 2008. Rupture of the medial gastrocnemius muscle during namaz praying: An unusual cause of tennis leg. Comput Med Imaging Graph, 32(8): 728-31. Abstract
Dr. Hossein, Dr. Cheng and Dr. Helman have no conflict of interest to declare
Now test your knowledge with a quiz.










[…] Cases features a discussion of commonly missed uncommon orthopedic injuries including syndesmotic injuries, bicep tears, quad/patella tears and gastroc tears. Great tips and […]
I was surprised by the ciprofloxin comment on the orthopaedic injury
?the source or was it a plant to see if we were following’
cheers
Since 1983 the use of floroquinolones have been associated with tendon rupture.
http://www.medscape.com/viewarticle/410546_3
I don’t think there is any hard evidence, just an association.
Anton
THank you very much. I am endocrinologist, but these are really useful to me
Khue