Welcome to the new EM Cases CritCases blog, a collaboration between Mike Betzner, the STARS air ambulance service and EM Cases’ Michael Misch and Anton Helman! These are educational cases with multiple decision points where there is no strong evidence to guide us. Various strategies and opinions from providers around the world are coalesced and presented to you in an engaging format. Enjoy!
Written by Michael Misch; Edited by Anton Helman; Expert Peer Review by Margaret Thompson, Medical Director of the Ontario Poison Control Centre and Vice President of the Canadian Association of Poison Control Centres. January 2016.
The Case:
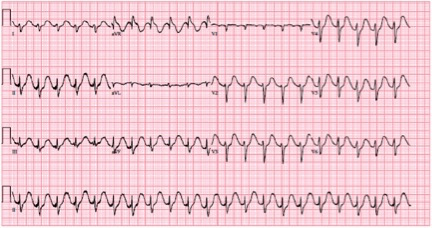
A 51-year old male presents to Janus General, a rural ED about 100 km from the nearest tertiary care centre. Five hours prior to presentation he ingested approximately 60 tablets of amitryptilline (50 mg tablets). Upon arrival in the ED he is confused and combative. Initial vital signs are BP 55/30 to 93/60, HR 135, RR 24, Temperature 37.4. Capillary glucose is normal. ECG is shown below.
What’s your interpretation of the this ECG? Is it typical for Massive TCA Overdose?
- Wide complex tachycardia (>120ms) with a right axis deviation
- Tall R wave in lead aVR
- QTc prolongation
The combination of these ECG findings is highly suspicious for a Sodium Chanel Blocker overdose, of which TCA is a classic example.
Case continued…
Following a 1L bolus of normal saline, he is given 2 amps of sodium bicarbonate (100 mEq) via IV bolus and an infusion of 3 amps (150 mEq) in 1000 mL of D5W at 250 mL/hr. Initial investigations are below:
| Na | 142 | Hb | 141 | pH | 7.3 | Acetaminophen | < 66 |
| K | 3.5 | Lk | 11.9 | pCO2 | 46 | Ethanol | 13 |
| Cl | 103 | Plt | 297 | HCO3 | 23 | Salicylates | < 0.07 |
| HCO3 | 22 | pO2 | 160 | ||||
| Cr | 65 | Lactate | 5.1 | ||||
| Glc | 6.3 | ||||||
| Urea | 5.4 | ||||||
His systolic blood pressure remains 50-80 mmHg. The QRS intermittently widens to greater than 160 ms and looks like ventricular tachycardia with repeated boluses of sodium bicarbonate causing transient narrowing of the QRS. Norepinephrine is started and rapidly titrated up to 0.4 mcg/kg/minute. The patient becomes increasingly agitated, requiring multiple doses of IV midazolam. He subsequently becomes unresponsive with a GCS of 3.
Care has been transferred to the transport team and the patient is en route by helicopter to the tertiary care centre, approximately 30 minutes away.
The patient has already received 200 mEq of sodium bicarbonate.
How much sodium bicarbonate is too much? Should you give more bicarbonate or move on to other therapeutic options for Massive TCA Overdose?
There are multiple proposed mechanisms to explain the benefit of sodium bicarbonate therapy in tricyclic antidepressant (TCA) overdose. The most commonly cited are:
- High sodium load counteracting the blockade of sodium channels
- Alkalization of the blood, which may decrease the proportion of unbound TCA available and may directly reduce the efficacy with which TCA binds to sodium channels
The evidence for sodium bicarbonate in TCA overdose consists largely of case reports and animal studies. However, the largest cohort study of TCA overdose used a max pH of 7.55 and most clinicians will target a pH of 7.50-7.55. Additionally, a serum sodium of 150-155 mmol/L is often cited as the upper limit for sodium bicarbonate use. Aside from these parameters there does not seem to be a predefined maximum dose. The regimen used in this case is commonly seen in practice: 100-150 mEq of sodium bicarbonate given IV push followed by 100-150 mEq in 1000 ml of D5W at 250 ml/hour. It is important to monitor electrolytes and blood gases, (some would suggest hourly) particularly looking for hypokalemia and alkalosis. A reasonable approach would be to give sodium bicarbonate as above, check your electrolytes and a blood gas. If you’ve reach a pH of 7.5-7.55 or a Na of 150-155 mmol/L then it is likely time to move on to your next option.
This case was tweeted out twice and garnered 3,306 impressions and 720 engagements. Many clinicians including EM physicians, toxicologists and critical care physicians voiced their opinions and many said that they would give more bicarb after 200mEq had been given without significant clinical or ECG improvement. However, David Juurlink (@DavidJuurlink) suggested that after 4 amps of bicarb with no clinical improvement, it was time to move on to other therapies.
Are you going to give intralipid now? Do you have it stocked in your ED?
While most evidence for use of intralipid (20% lipid emulsion) in poisoned patients is based on local anesthetic toxicity, it’s use should be considered for any lipophilic, cardiotoxic drug for which supportive therapies have failed. Intralipid is essentially TPN and is thought to act as a “lipid sink” that effectively reduces the level of free TCA in the blood. Intralipid has been studied for TCA overdose in animal models and described in several case reports. There is a well-described protocol at lipidrescue.org, which can be used as a point-of-care resource if need be. However, this is an opportune time to contact your local poison control centre to speak to an expert toxicologist to help guide management, if the situation permits. Intralipid is given as an initial bolus of 1.5 ml/kg (approximately 100 cc) over one minute followed by 0.25 ml/kg/hour, to a maximum dose of 12mL/kg. Given the increasing use of intralipid as a rescue antidote for several cardiotoxic medications including calcium channel blockers and beta-blockers, it is important to know whether it is stocked in your ED or not. In this scenario the patient was already en route via helicopter where intralipid was not available, and so intralipid was not an option until arrival at the tertiary care centre. Some EMS services in Canada do carry intralipid.
Chris Hicks (@HumanFact0rz) tweeted “Consider bumping upintralipid in the algorithm — not just a rescue treatment”
Salim Rezaie (@srrezaie) tweeted that in the emergency department where he works it takes time to obtain intralipid from the pharmacy and suggested early use of push dose pressors. This led to a conversation about intralipid availability in EDs and that intralipid should be available in all EDs for cases such as this.
Intralipid is not immediately available. What other medications are you going to try for Massive TCA Overdose?
Unfortunately, there are no evidenced-based algorithms to guide your next decision here and so there is no clear right answer in this scenario. Here are a few options to consider:
Hypertonic Saline (HTS)
In animal studies, hypertonic saline has been shown to have comparable effects to sodium bicarbonate with regards to improving blood pressure and QRS duration. Recall that the sodium load of sodium bicarbonate is a primary mechanism for its role as an antidote for TCA toxicity. While not first line, consider using it when a pH > 7.55 precludes the use of more sodium bicarbonate in a patient with persistent hypotension and in the setting of a wide QRS. While there is no dose-finding study to guide its use in this situation, consider the same dosing as you would for other indications: 100 ml of 3% HTS IV.
Lidocaine
While the use of a sodium channel blocker such as lidocaine in a TCA overdose may seem counterintuitive, it is thought to outcompete the sodium channel-blockade effects of a TCA. Unlike other anti-arrythmics, lidocaine will also not prolong the QT. Consider lidocaine in patients with dysrhythmias refractory to sodium bicarbonate, hypertonic saline or when alkalosis hypernatremia limits their use. Standard dosing for lidocaine applies in this situation: 1-1.5 mg/kg.
Vasopressors
Norepinephrine is increasingly the initial vasopressor of choice in patients with undifferentiated shock and it has also been found to be successful anecdotally in TCA overdose. The alpha-adrenergic properties of norepinephrine are suited to counteract the alpha-blockade mechanism of TCA toxicity. Theoretically, the beta-adrenergic effects of epinephrine may better counteract the cardiotoxic effects of TCAs and may be added if there is evidence of poor contractility on echo or hypotension refractory to norepinephrine. There is no clinical evidence to support this unfortunately.
Magnesium Sulfate
Magnesium sulfate can be considered for refractory ventricular dysrhythmias causing hemodynamic instability in TCA overdose, as TCAs can also block potassium channels. QT prolongation associated with TCA overdose may predispose to Torsades de Pointes, for which magnesium is sometimes indicated. In case studies, magnesium administration was associated with narrowing of the QRS and improved hemodynamics in patients with refractory ventricular dysrhythmias following TCA overdose. Consider standard ACLS dosing: 1-2 g IV over 15 minutes to start.
Case continued…
The patient is intubated by rapid sequence intubation with 0.3 mg/kg of etomidate and 1.2 mg/kg of rocuronium. A ketamine infusion is started for sedation. An orogastric tube is inserted and charcoal is given.
Dr. Andrea Boone “Does he even need sedation? GCS 3…Given he is paralyzed I would look for increasing tachycardia as an indicator for need for sedation.”
Dr. Jamie Fox “I would treat this patient with whole bowel irrigation as we may still be early enough to decontaminate the GI tract”
Dr. Mark Yarema “Lavage followed by charcoal, would be a good thought in the first hour or two. The benefit of lavage remains unclear, and there are reports of complications because it’s done so infrequently these days. TCA’s bind to charcoal readily, and the charcoal might be good enough. Certainly it would never be wrong to not lavage these patients. WBI is typically reserved for extended release preps or body packers. Mixing WBI and charcoal together actually might decrease the adsorptive capacity of charcoal because the PEG solution binds to it too, so would typically recommend just picking the charcoal, or at least separate the two procedures by several hours to let the charcoal pass (which probably defeats the purpose of WBI in the first place).
What ventilation strategy are you going to use in Massive TCA Overdose?
The patient should not be allowed to become acidemic. Given that alkalosis to a target of 7.50-7.55 can reduce the degree of sodium channel blockade in TCA overdose, consider mild hyperventilation with a target PaCO2 of 30-35. Initial ventilator settings might be: Assist Control Rate of 20, Tidal Volume of 8 cc/kg of ideal body weight, and an initial PEEP. Start FiO2 at 100% and rapidly titrate down to target an oxygen saturation of 95%.
Dr. Paul Tourigny “I would offer a slightly different take on ventilation: consider not only an open lung/lung protective strategy, but also remember to consider your minute ventilation. As a rough guide, non-intubated people have an Mv of ~60 cc/kg/min. The simple obtunded patient requiring intubation/ventilation requires about 120 cc/kg/min. People on death’s doorstep are requiring ~240 cc/kg/min. He is going to be sick with a fairly high metabolic demand and will likely require a higher minute ventilation. If he is 5’6″ tall, his tidal volume 8 cc/kg ideal body weight is ~488 cc. Call it 500 cc to make this an easy number and 20 breaths/min gives you a minute ventilation of 10 L. If you divide this by him IBW, this gives you an Mv of 164 cc/kg/min. This might be a little low for his metabolic demand and I might go a little higher on my rate. I’d watch for autoPEEP. I’d also do serial gases to track whether we were managing his acidosis and I’d titrate my rate to keep his pH around 7.5-7.55. Tracking pCO2 would be less helpful because of the amount of bicarbonate we’re giving him.”
Does Extra-Corporeal Membrane Oxygenation (ECMO) have a role in massive TCA overdose?
While ECMO may not be available in your department, case reports have described the use of ECMO in near-fatal TCA overdoses. One case report described an asystolic arrest requiring three hours of CPR following a multi-drug overdose including amytryptilline and carvedilol. The patient was placed on ECMO and survived to discharge without neurological sequelae. If you have it available, it’s a nice option to have in the refractory peri-arrest TCA overdose.
Case Resolution
While en route to the tertiary care centre, the patient’s MAP was maintained on a 0.4 mcg/kg/minute norepinephrine infusion. QRS duration remained approximately 160 ms with only a transient narrowing with each subsequent sodium bicarbonate bolus (an additional 4 ampules of 50 mEq are given during transport). Upon arrival at the tertiary care centre, the patient received intralipid with subsequent improvement in hemodynamics and QRS morphology. He received a total of approximately 300 mEq of sodium bicarbonate. Of note, the serum sodium was found to be 158 mmol/L and pH was 7.45 on arrival. Monitoring of electrolytes and blood gases would have helped to guide sodium bicarbonate therapy but was not possible during transfer. The patient was admitted to the ICU for two days with subsequent transfer to the psychiatry department neurologically intact.
Expert Peer Review by Margaret Thompson
Tricyclic anti-depressant (TCAs) medications are not used to the same extent for depression that they once were; there are other indications, and overdose, when seen, is a picture of depressed level of consciousness, seizures, dysrhythmias and hypotension, leading to death. There is no antidote; management is aggressive supportive care with some theoretical reasoning behind strategies chosen. A main mechanism by which this class of medications cause hypotension and dysrhythmias is fast sodium channel blockade of the action potential of smooth and cardiac muscle. Many other medications also have this “membrane stabilizing effect” as it might also be referred to in the literature. The important message is that the strategies used to treat the TCA overdose can be extrapolated in many other overdose situations… for the type 1A and 1C anti-dysrhythmics, cocaine, propranolol, anti-psychotics, anti-histamines in large amounts – to name a few.
The hallmark findings of sodium channel blockade are a wide QRS and an RR’ (or a positive terminal R wave) in AVR. There is some evidence that the QRS wider than 100 msec is predictive of seizures in a TCA overdose and wider than 160 msec of dysrhythmias. A bolus of 1-2mEq/kg (1-2 amps) of sodium bicarbonate should be given for a wide QRS in the setting of a sodium channel blocker overdose. If the QRS narrows, this bolus can be repeated if it were to widen out again. IF this initial bolus does not work, then another 1-2 mEq/kg (1-2 amps) can be given immediately. If 4 amps of sodium bicarbonate have been given with no response, it is probably prudent to give 100 mL 3% saline in an attempt to overcome the blockade (put in simple terms). As suggested by Dr. David Juurlink, there is some human evidence that this might work. One must monitor serum sodium (keep less than 155 maximum) and pH (maximum 7.5) using this treatment. There is no evidence that a bicarbonate infusion will be effective or prevent further widening of the QRS and is not recommended. Correcting acidosis is of benefit; in the acidemic environment, there may be better binding of tricyclics to cardiac sodium channels and lipid therapy is more effective at a neutral pH.
Tricyclics may block norepinephrine receptors, eventually leading to norepinephrine depletion; this provides theoretical evidence that norepinephrine would be the pressor of choice in the setting of TCA toxicity.
The position statement of the American College of Medical Toxicology regarding lipid emulsion therapy suggests a maximum of 2 full doses of 20% lipid. There are downsides to lipid therapy including pancreatitis, pulmonary lipid emboli as well as not being able to monitor patient status as electrolytes, gases etc. cannot be measured in such lipemic serum.
Intralipid treatment should be reserved for:
- Hypotension
- Dysrhythmias causing hemodynamic instability (not responsive to sodium bicarbonate or lidocaine) or
- Seizures unresponsive to usual treatments.
Take Home Points for Management of Massive TCA Overdose
- Use a QRS > 100 msec, a target pH of 7.5-7.55 and serum sodium of 150-155 mmol/L to guide sodium bicarbonate bolus therapy in TCA overdose. After 4 amps of sodium bicarbonate, if these targets are not met, consider adjunctive therapies.
- Intralipid (20% lipid emulsion) should be considered in hemodynamically unstable TCA overdose patients, those with refractory ventricular dysrhythmias following adequate sodium bicarbonate therapy or lidocaine, and those with refractory seizures.
- Adjunctive therapies for massive TCA overdose include hypertonic saline, lidocaine, magnesium sulfate and ECMO where available.
Other FOAMed Resouces on TCA Overdose & Intralipid Therapy
For more on Lipid Emulsion Therapy on EM Cases, Lisa Thurgur tells all on Episode 44 from The Whistler’s Update in EM Conference
TCA Toxicity on Life in the Fast Lane
TCA Oversode on EMCrit
References
Body R, Bartram T, Azam F, Mackway-jones K. Guidelines in Emergency Medicine Network (GEMNet): guideline for the management of tricyclic antidepressant overdose. Emerg Med J. 2011;28(4):347-68.
Blackman K, Brown SG, Wilkes GJ. Plasma alkalinization for tricyclic antidepressant toxicity: a systematic review. Emerg Med (Fremantle). 2001;13(2):204-10.
Citak A, Soysal DD, Uçsel R, Karaböcüoğlu M, Uzel N. Efficacy of long duration resuscitation and magnesium sulphate treatment in amitriptyline poisoning. Eur J Emerg Med. 2002;9(1):63-6.
Deegan C, O’brien K. Amitriptyline poisoning in a 2-year old. Paediatr Anaesth. 2006;16(2):174-7.
Foianini A, Joseph wiegand T, Benowitz N. What is the role of lidocaine or phenytoin in tricyclic antidepressant-induced cardiotoxicity?. Clin Toxicol (Phila). 2010;48(4):325-30.
Hoffman JR, Votey SR, Bayer M, Silver L. Effect of hypertonic sodium bicarbonate in the treatment of moderate-to-severe cyclic antidepressant overdose. Am J Emerg Med. 1993;11(4):336-41.
Koschny R, Lutz M, Seckinger J, Schwenger V, Stremmel W, Eisenbach C. Extracorporeal life support and plasmapheresis in a case of severe polyintoxication. J Emerg Med. 2014;47(5):527-31.
Mccabe JL, Cobaugh DJ, Menegazzi JJ, Fata J. Experimental tricyclic antidepressant toxicity: a randomized, controlled comparison of hypertonic saline solution, sodium bicarbonate, and hyperventilation. Ann Emerg Med. 1998;32(3 Pt 1):329-33.
Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S729-67.
Ozcan MS, Weinberg G. Intravenous lipid emulsion for the treatment of drug toxicity. J Intensive Care Med. 2014;29(2):59-70.
Sarisoy O, Babaoglu K, Tugay S, Barn E, Gokalp AS. Efficacy of magnesium sulfate for treatment of ventricular tachycardia in amitriptyline intoxication. Pediatr Emerg Care. 2007;23(9):646-8.
Seger DL, Hantsch C, Zavoral T, Wrenn K. Variability of recommendations for serum alkalinization in tricyclic antidepressant overdose: a survey of U.S. Poison Center medical directors. J Toxicol Clin Toxicol. 2003;41(4):331-8.
Tran TP, Panacek EA, Rhee KJ, Foulke GE. Response to dopamine vs norepinephrine in tricyclic antidepressant-induced hypotension. Acad Emerg Med. 1997;4(9):864-8. Full PDF
Williams JM, Hollingshed MJ, Vasilakis A, Morales M, Prescott JE, Graeber GM. Extracorporeal circulation in the management of severe tricyclic antidepressant overdose. Am J Emerg Med. 1994;12(4):456-8.
Dr. Helman, Dr. Misch, Dr. Betzner & Dr. Thompson have no conflicts of interest to declare





I received the following questions directly from a reader:
Nice!!!! Some thoughts and questions below:
Do you know what vent settings the patient ended up with?
Dr Tourigny vent strategy is interesting. I agree with his minute ventilation, likely a higher rate would benefit the patient.
As for sedation, definitely needed, along with an analgesic. Pt comfort will decrease their metabolic demand, O2 consumption and agitation. Possibly improving some of the tachycardia. Making it safer in flight for patient and crew.
Glad to hear Lipids were used. Does the helicopter carry? Could you have picked up enroute if not?
Whole bowel irrigation: Not sure I have ever seen done in our ER? As for charcoal, did the patient receive on her arrival to hospital? Or only once at Tertiary centre? What is effectiveness if greater than an hour post ingestion?
Fluids: patient received one bolus, did they receive additional fluids? Or, did you switch to norepi for sole BP control? Not sure that I worded that correctly, but wondered about urine output and its concentration. Would fluids have helped flush the TCA?
Interesting case for sure, thank you for sharing!
My responses were as follows:
A patient like this would settle out on 18 X 500 on the vent with a goal pH obtained of 7.5.
In super sick patients like this, I would personally sedate for the trip with a ketamine infusion alone. I would not add other agents as the propensity for sudden hemodynamic compromise is so high in a patient like this.
Most helicopters do not carry intralipids. It is an upload item from most rural hospitals though and or certainly from tertiary care if a flight MD is being picked up.
I would not WBI a patient like this. I would lavage and charcoal if within 90 minutes personally. Charcoal alone if longer. This patient got charcoal in the sending community. I would intubate 1st if any alteration in LOC. I generally wouldn’t give at all if longer than 4 hours post ingestion. Effectiveness of course declines with time, but given TCAs have such significant anticholinergic properties, gut emptying will be delayed.
The patient did not receive additional fluids beyond that required for the NaHCO3 boluses and to run the bicarb infusion. I also do not personally run bicarb infusions in these kinds of patients, but generally will run 1.5X maintenance NS + will alkalinize using the vent. Fluids do not help flush the TCA. They are predominantly hepatically metabolized as well as excreted in the urine to a lesser degree.
These patients are not generally dehydrated significantly when they are relatively fresh in the overdose. NorEpi helps replace the NorEpi depletion caused by the fact TCAs block the reuptake of NorEpi, which then allows the MAOi system to metabolize all the intrinsic NorEpi until there is none left.
Mike
[…] Helman reviews a case of massive TCA toxicity and discusses use of sodium bicarbonate and intralipid therapy. […]
Great case based discussion. Thanks.
Cost of intralipid is minimal, here in the UK £10 per 100ml bag (~US$16-20). It has a long shelf life and forms part of our standard antidote stock in EDs.
Hello dr Anton Any way we can surf through podcasts. Tried to bring this with the low and slow but couldn’t
Is there any option to group different podcasts under different specialties or pathologies ie toxico cases under toxicology etc
Nice case report and practically useful! Thanks
this is an excellent case and review. The crowdsourcing and expert opinion format is a great approach. thank you