In this EM Cases main episode podcast Occult Shoulder Injuries and Proximal Humerus Fractures, Dr. Arun Sayal and Dr. Dale Dantzer answer questions such as: What should be included in the list of key occult shoulder injuries that we should have in our back pockets when faced with a patient who has injured their shoulder and the x-ray appears normal? Which proximal humerus fractures are likely to require surgical management? Which shoulder injuries require a simple sling vs Velpeau sling vs collar and cuff vs sugar tong splint? When is an ultrasound of the shoulder indicated and how should they be interpreted? What is the best x-ray view to diagnose a sternoclavicular dislocation? What are the surgical indications for clavicle fractures? and many more…
Podcast: Play in new window | Download (Duration: 49:04 — 44.9MB)
Subscribe: Apple Podcasts
Podcast production, sound design & editing by Anton Helman
Written Summary and blog post by Saswata Deb, edited by Anton Helman February, 2020
Cite this podcast as: Helman, A. Sayal, A. Dantzer, D. Episode 136 Occult Shoulder Injuries and Proximal Humerus Fractures. Emergency Medicine Cases. February, 2020. https://emergencymedicinecases.com/occult-shoulder-injuries-proximal-humerus-fractures. Accessed [date]
ED management of proximal humerus fractures
Surgery for proximal humerus fractures offer little benefit over conservative for the vast majority of proximal humerus fractures [1,2,3] and is associated with increased costs, adverse event rates, and risk of mortality [4]. There is geographical variation in the proportions of patients that undergo surgical management of proximal humerus fractures with rates ranging from 9%-21% [5].
There are four general considerations in the decision for surgical management of these fractures: The Neer classification suggest that the more bone fragments, the more likely surgery will benefit the patient [6]. Furthermore, the more displaced the humeral head, the more likely avascular necrosis may result (although AVN in rare), and the more likely a benefit from surgery. Greater tuberosity fractures that displace proximally enough to disrupt the joint usually require surgery, and head split fractures usually require surgery.

Neer classification proximal humerus fractures, University of Washington
Patients should be made aware that about 90% of recovery of the shoulder from proximal humerus fractures occurs in the first 3-4 months and the remaining 10% takes 6 months or longer – much longer than other major joints in the body [7]. In addition, simple range of motion exercises such as pendulum swings and wall walk-ups should be encouraged and can be quickly demonstrated in the ED. These exercises help to prevent adhesive capsulitis (frozen shoulder).
Pitfall: Patients with proximal humerus fractures who are instructed to remain immobilized for more than three weeks are put at increased risk for adhesive capsulitis. Early range of motion exercises are key in preventing frozen shoulder.
Methods of shoulder immobilization
There are 4 ways to immobilize the shoulder: simple sling, Velpeau sling (‘shoulder immobilizer’), collar and cuff and sugar tong splint.
The simple and Velpeau slings take the weight of the arm off the shoulder. In patients with clavicular fractures or acromio-clavicular (AC) separations, such slings that take the weight off the shoulder help to relieve pain and may promote healing. In contrast, sugar tong splints and cuff and collar take advantage of the weight of the arm and the resulting force of gravity that provides axial traction to the fracture. For patients with impacted proximal humerus fractures, a sugar tong may be beneficial to align the fracture fragments, while for patients with displaced/angulated midshaft humerus fractures a sugar tong splint may promote reduction of the fracture.
Occult shoulder injuries: those with a normal appearing x-ray or subtle findings
There are 6 significant shoulder injuries which often have subtle or no specific findings on x-ray that one should consider:
- Posterior shoulder dislocation (Episode 135)
- Glenohumeral subluxation
- Rotator cuff injuries
- AC separation
- Sternoclavicular subluxation/dislocation
- Occult pediatric clavicle fracture
Glenohumeral subluxation
Glenohumeral subluxations are typically seen after a sports injury or in young females with a history of hypermobility [8]. Patients may report that they felt like their shoulder move out of place and then “pop back in”.
The apprehension test and relocation tests confirm the diagnosis of glenohumeral subluxation – the caveat being the patient who has dislocated their glenohumeral joint recently where the test may be falsely positive [9]. There is little value in doing this test if dislocation occurred within a few weeks of presentation.
Treatment is immobilization in a sling in the position opposite to the mechanism of injury. For anterior subluxation, immobilize with the shoulder internally rotated (forearm against the abdomen); for posterior subluxation, immobilize in an external rotation shoulder brace with the shoulder in 10-15 degrees of external rotation.

External rotation shoulder brace for immobilization of reduced posterior glenohumeral subluxation or dislocation
Rotator Cuff Injuries: Difficult to diagnose clinically or with ultrasound
There are 3 types of pathology to consider in rotator cuff injuries. These include rotator cuff tendonitis, acute rotator cuff tear, and chronic rotator cuff tear.
The most common mechanism for an acute rotator cuff tear is forceful abduction against resistance, with attempt to lift heavy object as another common mechanism of injury. Patients may report a sudden tearing sensation followed by severe pain radiating into the arm.
Traditional teaching dictates that patients with acute full rotator cuff tears are unable to initiate abduction and that the drop-arm test (patient’s arm is held in 90 degrees abduction and let go resulting in an abrupt drop to the side) is very accurate for the diagnosis of acute rotator cuff tear. However, while some studies have suggested that various combinations of historical and physical examination findings are highly accurate in diagnosing rotator cuff tears [10], while others have found only moderate diagnostic accuracy with low prediction value for prediction models [11], our experts believe that there is no finding or combination of findings on history or physical that can accurately diagnose rotator cuff tear in the acute setting. While it may be tempting to order an ultrasound in the ED, many patients over the age of 60 will have pre-existing rotator cuff abnormalities (including chronic bilateral full thickness tears) found on ultrasound and it is very rare that any of them will require surgery. The quality of ultrasound reporting is also highly variable and there are many false positives with sensitivities and specificities of 89% and 84% respectively[12]. Our experts suggest that in the ED, U/S of the shoulder is rarely required, as most of the time, the management is non-surgical. Refer only young patients with highly suspected acute rotator tear and arrange outpatient ultrasound for confirmation.
Acromioclavicular (AC) separation
The mechanism of an AC separation is typically a fall on to the tip of shoulder (direct blow to the lateral acromion) with the arm adducted [13]. On exam there is tenderness with or without a prominence at the AC joint.
While the diagnosis is usually obvious from the history and physical, x-rays are nonetheless indicated to rule out a distal clavicle fracture. Place a sling on the patient for comfort before sending them for x-rays. X-rays with weights are no longer recommended, however, it is recommended to obtain bilateral x-ray views to compare the acromioclavicular distance of the normal to the injured side. While there are numerous classifications systems described, a simple rule of thumb for consideration of surgical intervention is if the AC distance is increased 100% or 5mm on the injured side compared to the normal side – referral to orthopedics for consideration of surgery is advised [14].
Sternoclavicular (SC) subluxation/dislocation
Anterior SC dislocation (90% of all SC dislocations) is usually the result of a direct blow to anterolateral shoulder, which levers the proximal clavicle anteriorly, while posterior SC subluxation is usually the result of a direct blow to the posterolateral shoulder (rather than the rarer direct blow to the proximal clavicle mechanism) [15]. This is why we should always systematically start the shoulder exam at the SC joint.
Posterior SC dislocation can be life-threatening due to the structures that lie beneath the SC joint. Potential injuries include a pneumothorax, tracheal, esophageal, neurologic (brachial plexus) or vascular (subclavian vein) injury. It is not always obvious on physical exam if the dislocation/subluxation is anterior or posterior as there is usually significant swelling and tenderness at the SC joint. Some clinical clues to the dreaded posterior dislocation are a hoarse voice, difficulty swallowing, SOB, cyanosis, weak/numb arm from brachial plexus injury.
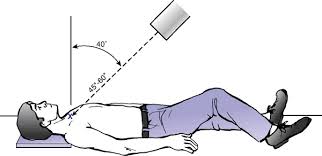
Serendipity view is the view of choice for SC subluxation/dislocation where an anterior subluxation would appear superior on the film and a posterior subluxation would appear inferior. Even these are difficult to interpret, and many patients end up needing a CT scan, which is advised for all suspected posterior dislocations to assess the integrity of vital structures beneath.

Serendipity view x-ray to assess for sternoclavicular dislocation/subluxation
Reduction may be attempted in the ED for anterior SC dislocations, but because the stable structures around the dislocated joint are damaged, re-dislocation occurs frequently after reduction [15]. The reduction technique involves procedural sedation followed by placing a bolster between the shoulders of the supine patient. Next, traction is applied to the arm in 90 degrees of abduction and a direct downward force is applied over the medial clavicle. Posterior dislocations are best reserved for the OR with thoracics back up in the event that a blood vessel that is damaged (but tamponaded by the clavicle) bleeds as a result of the reduction, and for any repair to thoracic organs that may be required [16].
Pediatric occult clavicle fracture
The x-ray of a child with a mid-clavicle fracture may appear normal [17]. If a child presents after a fall onto the adducted shoulder, with pain and tenderness over the mid-clavicle, they should be treated as an occult clavicle fracture with a shoulder sling and follow up.
Learn more about pediatric fractures at Ep 35: Pediatric Orthopedics Pearls and Pitfalls
Which adult patients with clavicle fractures should be referred for consideration of surgery?
Patients who undergo surgery for middle-third clavicle fractures have a lower incidence of nonunion and symptomatic malunion, however functional outcomes are similar to non-surgical treatment, and complication rates are higher in those that undergo surgery [18].
Four indications for referral to orthopedics for an adult with a clavicular fracture for surgical consideration include:
- Mid-clavicle fracture with shortening ≥2cm
- Distal 1/3 clavicle fracture or displaced medial 1/3 clavicle fracture
- The presence of skin tenting or open fracture
- Neurovascular injury
Pearl: For a fracture that causes tenting of the skin, apply a surgical prep (sterile dressing) in case it converts to an open fracture while awaiting surgery.
Figure of 8 bandages are no longer recommended for treatment of clavicle fractures [19]. A simple sling or Velpeau sling is the immobilization technique of choice.
Learn more about shoulder injuries at Ep 135: Commonly Missed or Mismanaged Shoulder Injuries- Approach and Glenohumeral Dislocations
References
- Fu T, Xia C, Li Z, Wu H. Surgical versus conservative treatment for displaced proximal humeral fractures in elderly patients: a meta-analysis. Int J Clin Exp Med. 2014;7(12):4607-15.
- Xie L, Ding F, Zhao Z, Chen Y, Xing D. Operative versus non-operative treatment in complex proximal humeral fractures: a meta-analysis of randomized controlled trials. Springerplus. 2015;4:728.
- Rangan A, Handoll H, Brealey S, Jefferson L, Keding A, Martin BC, et al. Surgical vs nonsurgical treatment of adults with displaced fractures of the proximal humerus: the PROFHER randomized clinical trial. JAMA. 2015 Mar 10. 313 (10):1037-47.
- Floyd SB, Thigpen C, Kissenberth M, Brooks JM. Association of Surgical Treatment With Adverse Events and Mortality Among Medicare Beneficiaries With Proximal Humerus Fracture. JAMA Netw Open. 2020;3(1):e1918663.
- Floyd SB, Campbell J, Chapman CG, Thigpen CA, Kissenberth MJ, Brooks JM. Geographic variation in the treatment of proximal humerus fracture: an update on surgery rates and treatment consensus. J Orthop Surg Res. 2019;14(1):22.
- Carofino BC, Leopold SS. Classifications in brief: the Neer classification for proximal humerus fractures. Clin Orthop Relat Res. 2013;471(1):39-43.
- Torrens C, Corrales M, Vilà G, Santana F, Cáceres E. Functional and quality-of-life results of displaced and nondisplaced proximal humeral fractures treated conservatively. J Orthop Trauma. 2011 Oct. 25 (10):581-7.
- Gil JA, Defroda S, Owens BD. Current Concepts in the Diagnosis and Management of Traumatic, Anterior Glenohumeral Subluxations. Orthop J Sports Med. 2017;5(3):2325967117694338.
- Lizzio VA, Meta F, Fidai M, Makhni EC. Clinical Evaluation and Physical Exam Findings in Patients with Anterior Shoulder Instability. Curr Rev Musculoskelet Med. 2017;10(4):434-441.
- Cadogan A, Mcnair P, Laslett M, Hing W, Taylor S. Diagnostic accuracy of clinical examination features for identifying large rotator cuff tears in primary health care. J Man Manip Ther. 2013;21(3):148-59.
- Van kampen DA, Van den berg T, Van der woude HJ, et al. The diagnostic value of the combination of patient characteristics, history, and clinical shoulder tests for the diagnosis of rotator cuff tear. J Orthop Surg Res. 2014;9:70.
- Smith TO, Back T, Toms AP, Hing CB. Diagnostic accuracy of ultrasound for rotator cuff tears in adults: a systematic review and meta-analysis. Clin Radiol. 2011;66:1036–1048.
- Warth RJ, Martetschläger F, Gaskill TR, Millett PJ. Acromioclavicular joint separations. Curr Rev Musculoskelet Med. 2013;6(1):71-8.
- Sirin E, Aydin N, Mert topkar O. Acromioclavicular joint injuries: diagnosis, classification and ligamentoplasty procedures. EFORT Open Rev. 2018;3(7):426-433.
- Macdonald PB, Lapointe P. Acromioclavicular and sternoclavicular joint injuries. Orthop. Clin. North Am. 2008 Oct;39(4):535-45, viii.
- Morell DJ, Thyagarajan DS. Sternoclavicular joint dislocation and its management: A review of the literature. World J Orthop. 2016;7(4):244-50.
- Alao D, Guly HR. Missed clavicular fracture; inadequate radiograph or occult fracture?. Emerg Med J. 2005;22(3):232-3.
- Lenza M, Buchbinder R, Johnston RV, Ferrari BA, Faloppa F. Surgical versus conservative interventions for treating fractures of the middle third of the clavicle. Cochrane Database Syst Rev. 2019;1:CD009363.
- Andersen K, Jensen PO, Lauritzen J. Treatment of clavicular fractures. Figure-of-eight bandage versus a simple sling. Acta Orthop Scand. 1987;58:71-74.
Drs. Helman, Sayal and Dantzer have no conflicts of interest to declare
Now test your knowledge with a quiz.





Leave A Comment