Burn and inhalation injury patients present to the ED more often than one might think, with a staggering half a million annual visits in the USA alone. It turns out that for all burn patients—from minor to severe—there is a lot of room for improvement in ED management, counselling and disposition. Things like inaccurate estimation of burn size, unnecessary endotracheal intubation, over- and under-estimation of fluid resuscitation volumes, inadequate analgesia and inappropriate wound dressings are just some of the issues where a small change to ED practice patterns could have a huge impact on patient care. In this EM Cases main episode podcast we have the director of the Burn Unit at Hospital for Sick Children, Dr. Joel Fish and EM educator Dr. Maria Ivankovic discuss dozens of pearls and pitfalls in the management of both pediatric and adult burn and inhalation injuries management with a special appearance by airway master George Kovacs to talk about awake intubation in the burn and inhalation injuries patient…
Podcast: Play in new window | Download (Duration: 1:44:43 — 95.9MB)
Subscribe: Apple Podcasts
Podcast production, sound design & editing by Anton Helman
Written Summary and blog post by Shaun Mehta, edited by Anton Helman and Maria Ivankovic, May, 2019
Cite this podcast as: Helman, A. Fish, J. Ivankovic, M. Kovacs, G. Burn and Inhalation Injuries: ED Wound Care, Resuscitation and Airway Management. Emergency Medicine Cases. May, 2019. https://emergencymedicinecases.com/burn-inhalation-injuries/. Accessed [date]
Go to part 2 of this 2-part podcast on burn, inhalational, and electrical injuries
Always Consider Non-accidental Trauma in The Pediatric Burn Injury Patient
For the pediatric patient presenting with burn and inhalation injuries, always consider non-accidental injury in your differential, particularly when:
- Delayed presentation to care
- Story and injury pattern mismatch
- Burns with well-demarcated lines (e.g. immersion burn)
- Patterned burns (feet, hands or buttocks)
- Burns in a certain shape (e.g. iron, cigarette)
Learn more about pediatric non-accidental trauma in Episode 108
First Aid for Burns
What not to do: ice causes severe vasoconstriction and can even deepen the burn. Toothpaste is also harmful given the effects of fluoride.
What to do: run cold water for at least 20 minutes. Evidence suggests that this can reduce pain and edema, reduce the depth of the burn, decrease the overall inflammatory response, improve the speed of wound healing, and minimize scarring.
Managing Burn-Associated Pain

Pediatric burn pain management
Pain management should be a priority: Treating pain early and aggressively has been shown to prevent psychological trauma and even to improve healing. A multi-modal analgesic approach is recommended. Have a low threshold to include a narcotic given the severity of pain associated with burns. For pediatric burn patients, intranasal fentanyl and ketamine have similar analgesic effects, but fentanyl is preferred given greater rates of sedation and dizziness with ketamine.
Burn Classification: Don’t Use 1st, 2nd, 3rd Degree
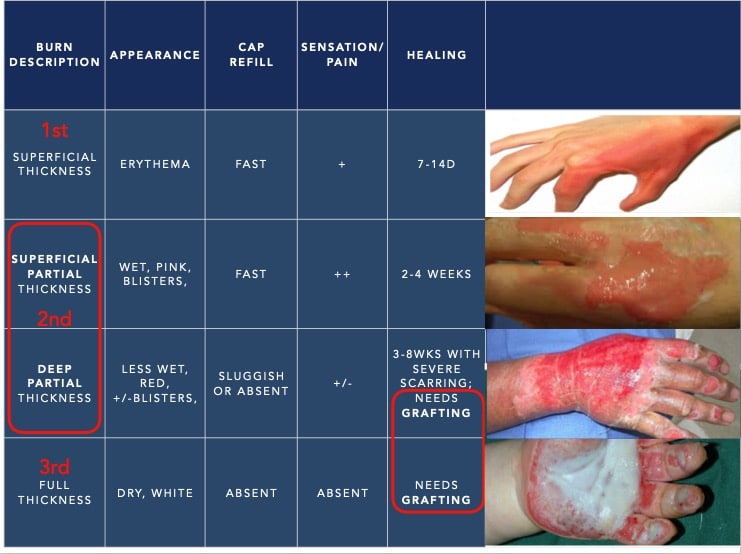
The burn classification system has moved away from the traditional 1st, 2nd and 3rd degree nomenclature to a more physiologic classification: superficial thickness, partial thickness (superficial vs. deep) and full thickness.
There are three anatomic layers of the skin important for burns:
- Epidermis: <1 mm in most areas, very thin layer of protection against bacteria and moisture loss.
- Dermis: the “brains” of the skin containing most of the functional elements such as nerves, sweat glands, hair follicles and blood vessels.
- Subcutaneous tissue
Many of the skin’s structures are protein-based which coagulate upon heat exposure in a burn injury. As the heat penetrates deeper into the skin, more functional structures are affected.
A superficial thickness burn involves the epidermis only and looks like a sunburn. The skin is erythematous and mildly painful, with a brisk cap refill.
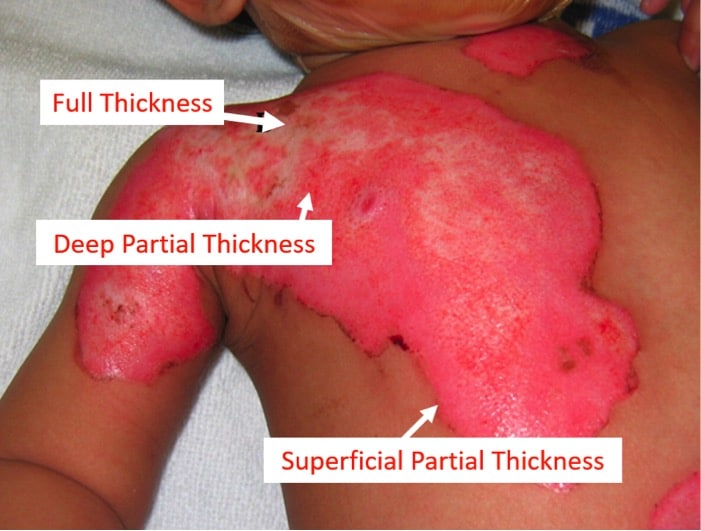
A superficial partial thickness burn goes beyond the epidermis to include the superficial dermis. These burns can have blisters, look wet, tend to be more painful but still have a fast cap refill time. Healing typically takes 2-4 weeks.
A deep partial thickness burn or deep dermal burn goes beyond the superficial dermis to include the deep dermis. These burns can look cherry red or pale and have sluggish cap refill. They may be less painful as more nerves have been destroyed. Healing may take 6 weeks and they generally require grafting to minimize scar and expedite healing.
A full thickness burn involves all layers of the skin and subcutaneous tissue, with involvement of underlying fascia, muscle and bone. They often look white or waxy or brown and leathery. There is no cap refill and they are usually painless in the immediate area. Treatment is always surgical.
PEARL: A superficial thickness burn will often disappear 3-4 hours after the event. If it remains, this burn may be a superficial partial thickness burn.
Burn Assessment Pitfalls
Do not use pain to exclude a full thickness burn. Burns are often mixed-depth and the edges of a full thickness burn can still be painful.
Both deep partial and full thickness burns may not blanch.
Burns are dynamic wounds. Burns can deepen over the next few days, and so it is difficult to know the true depth of the wound for at least 48-72 hours. Even burn specialists are only correct about 60% of the time at accurately identifying the depth of the burn on initial assessment. Burns can deepen after the first few hours to days of assessment. This is particularly important when setting expectations with patients and families at the initial visit.
PEARL: Burns in the ED are not easily classifiable on the initial assessment and they may convert to deeper burns over the next few days. Use caution when classifying burns and counseling patients and families about prognosis. Patients require close follow up of the wound for reassessment and ongoing care.
Classic example of a burn converting to full thickness from day 2-5, courtesy of Dr. Joel Fish
Burn Size Estimation
Calculating Total Body Surface Area (TBSA) is crucial in determining initial fluid resuscitation and potential disposition. The Rule of 9s is inaccurate and consistently overestimates TBSA by about 20% which can lead to over-resuscitation.
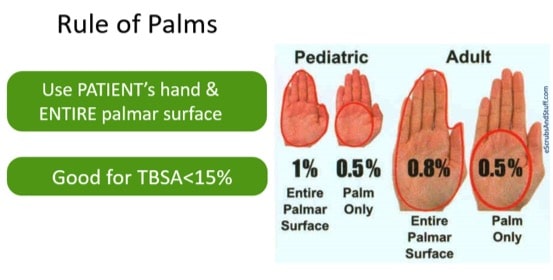
For TBSA <15% or >85%: The Rule of Palms is highly accurate and easy to teach. Use the size of the patient’s hand (including the fingers) to estimate burn size.
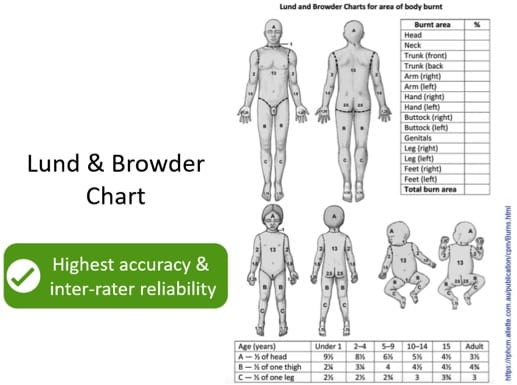
For TBSA >15%: The Lund & Browder Chart is accurate and has excellent inter-rater reliability.
Beware: Do not include superficial thickness burns in TBSA estimation. Only include partial and full thickness burns.
Wound Care in Burn Injuries
Clinical Pearls
Keep wounds moist. A moist environment promotes re-epithelialization and prevents cellular dehydration.
Use a Non-adherent Dressing. Use a dressing such as Mepitel, Jelonet or Adaptic that will cause less pain upon removal. Apply a petrolatum-based antibiotic ointment to the dressing (rather than the wound itself), then place the dressing over the wound.
The daily dressing is dead. The patient does not need to return to the ED for daily dressing changes. The initial non-adherent dressing can be left on for 2-3 days until the patient has their follow up appointment.
Don’t use silver sulfadiazine (Flamazine). Silver sulfadiazine may delay wound healing and requires more frequent dressing changes. Silver sulfadiazine creates a pseudoeschar around the wound that can also foster microbial colonization.
For burns that require cleaning use sterile water and a gentle soap. With a soapy washcloth very gently wipe but do not scrub the wound. For dirtier wounds use chlorhexidine. Avoid iodine as it is cytotoxic.
Burn Injuries Blisters – to debride or not to debride?
Although evidence is weak for debridement, our experts recommend debridement for the following reasons:
- They can restrict function
- They prohibit proper assessment of the wound
- Blister skin is dead; non-viable tissue is a source of infection and should be removed
- Dressings need to be in contact with the viable tissue which is not possible with intact blisters
- Blister fluid may deepen the burn
Blisters <6mm in diameter may be left intact. To debride a blister snip the top with scissors to de-roof it then use tissue forceps to debride the devitalized tissue.”
Learn more about burn blister debridement in EM Quick Hits 9
Resuscitation of the Burn and Inhalation Injuries Patient
One of the most important principles to remember with any burn patient is that they are a trauma and toxicology patient first. Don’t get distracted by the burns. Perform your primary and secondary survey as you normally would with a trauma patient and address the burns later.
Most common injuries associated with burns:
- Fractures (50-60%)
- Traumatic brain injury (20-25%)
- Thoracic or abdominal injuries (4-24%)
Carbon monoxide (CO) and cyanide poisoning are also associated with burn injuries. Apply 100% O2 to reduce the half-life of carboxyhemoglobin to all patients with a history of exposure to fire in an enclosed space.
PEARL: All burn patients are trauma and toxicology patients until proven otherwise.
Update 2021: Single academic trial (Korea) of 706 patients, found that patients who received hyperbaric oxygen therapy (HBO2) within 6 hours of carbon monoxide (CO) poisoning had a better 6-month neurocognitive prognosis with fewer poor outcomes compared to those treated between 6-24 hours. Abstract
Airway Considerations in the Burn and Inhalation Injuries Patient
The mortality of inhalational injuries is 10-30% and increases with greater TBSA burns. Be particularly suspicious of a significant inhalational injury if the patient or first responders report the patient was in an enclosed space for a minute or more.
While it is critical to anticipate impending airway compromise and consider securing an airway sooner rather than later, the systematic reviews suggests that 1/3 of burn patients are unnecessarily intubated in the ED. Signs such as singed nasal hairs and facial burns alone are not indications for intubation. Mild inhalational injuries in patients with normal oxygen saturations and no signs of respiratory distress can be safely observed.
| Indications for early intubation |
| Signs of respiratory distress, stridor, accessory muscle use |
| New onset of hoarseness |
| Blisters or edema of oropharynx |
| Deep burns to lower face or neck |
Tip: You can use a nasopharyngoscope to take a look at the airway. If the supraglottic area appears beefy red and sooty prepare for intubation soon but if it looks good that is reassuring. You could also use video laryngoscope to look for edema, charred mucosa or soot.
When intubating choose an ET tube size 7.5 or larger as smaller sizes may prohibit passage of a bronchoscope for later assessment. Using a very large tube can worsen airway edema.
PEARL: In the intubated burn patient, re-check the tube position frequently. Fluid resuscitation and edema can result in tube displacement.
A note on awake intubation – Dr. George Kovacs
- The key is meticulous topicalization
- Warn the patient and your team that topicalization may cause a subjective feeling of respiratory distress when the cords are anesthetized
- Acknowledge the risk of laryngospasm and be prepared to manage
- Performing awake intubation successfully requires repeated simulated deliberate practice
Equipment:
- Tongue depressors x 2 + 5% lidocaine ointment
- Atomizer + 4% aqueous lidocaine
- Crash airway kit and RSI equipment
- +/- Anxiolytic medication (e.g. 0.5-1.0 mg midazolam)
- Flexible laryngoscope (or video laryngoscope)
Steps:
- Trap the patient’s tongue with gauze and spray inside the mouth with 10cc of 4% lidocaine for 3-4 seconds
- Place tongue depressor with 5% lidocaine ointment smeared on the end on the posterior third of the tongue and let the lidocaine ointment melt onto the tissues; repeat 3 times for about 15-20 seconds for each application moving side to side to ensure the posterior third is well covered with the ointment
- Attempt to perform laryngoscopy (ideally with flexible laryngoscope or with video laryngoscope)
- If unable to do #3 due to patient gag, administer atomized lidocaine via nasal passage, 3 sprays x 3 times; repeat ointment administration as needed
For videos and in depth discussion on awake intubation read Dr. Kovacs’ free open access airway book (infinity edition)
Dr. Kovacs’ masterclass talk at ResusTO on Awake Intubation
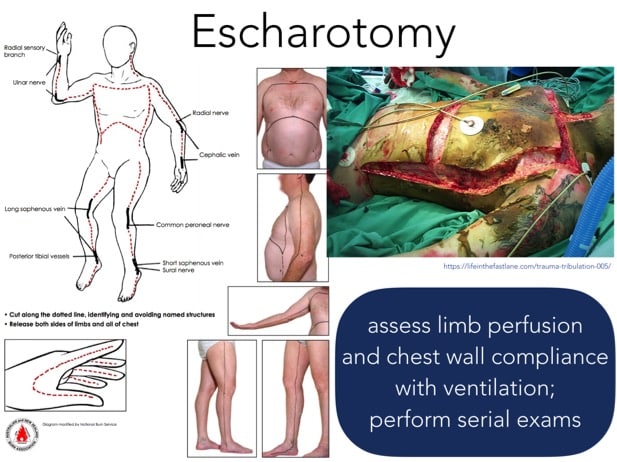
Indications for ED Escharotomy
Burns do not have to be circumferential to cause a compartment syndrome or restrict ventilation. Escharotomies are typically performed by a burn surgeon prophylactically to reduce the risk of compartment syndrome. If escharotomy is required immediately in the ED, call for help. Consider sending the burn surgeon a picture of the at-risk area and asking them to draw on a picture where to cut. The indications for ED escharotomy include:
- Inability to adequately ventilate due to restriction from chest eschar
- Absent or decreased pulses
- New neurologic deficits
In contrast to a fasciotomy that extends to deeper tissues, an escharotomy only includes the burned skin or eschar. It is ideally performed with cautery due to the risk of excessive bleeding with a scalpel. If using a scalpel, anesthetize using lidocaine with epinephrine to minimize bleeding. Do not extend the incision beyond the eschar. Incise mid-lateral and mid-medial areas of the limb to avoid neurovascular structures.
Cyanide Poisoning in Burn and Inhalation Injuries
Cyanide poisoning is a clinical diagnosis. Patients may present with non-specific symptoms similar to CO poisoning (nausea, headache, confusion). Suspect cyanide poisoning in patients exposed to a fire in an enclosed space and treat on speculation if:
- Altered mental status + soot in the mouth/nose (60% likelihood of CN poisoning)
- Altered mental status plus soot in the mouth/nose + hypotension/cardiac arrest (80% likelihood of CN poisoning)
Cyanide levels may take days to be resulted and is typically not recommended. Labs highly suspicious for CN poisoning include an anion gap metabolic acidosis or a lactate >8.
Consider treating cyanide poisoning on speculation if your burn patient has:
- Altered mental status (not attributed to head injury) + soot in the mouth or nose (portents about a 60% chance of cyanide poisoning)
- Altered mental status (not attributed to head injury) + soot in the mouth or nose + unexplained hypotension (portents about an 80% chance of cyanide poisoning)
Cyanide poisoning may present with non-specific symptoms similar to CO poisoning (nausea, vomiting, headache, confusion). Other features that should increase your suspicion of cyanide poisoning include burn in an enclosed space or with textiles/plastics, or an unexplained anion gap metabolic acidosis or lactate > 8.
Treatment of suspected cyanide poisoning
The antidote is hydroxocobalamin (Cyanokit) 5g given over 15min. Repeat the dose if the patient’s GCS, hypotension or dysrhythmia is not improving in 15 minutes. Give sodium thiosulfate in addition to the hydroxocobalamin (cyanokit).
Hydroxocobalamin is generally safe. Side effects include red urine, red skin, hypertension, nausea, decreased lymphocytes, injection site reactions, and (rarely) acute renal failure. It may interfere with lab tests so consider drawing labs quickly as the antidote is being prepared (but do not delay treatment).
Older cyanide antidote kits contain sodium thiosulfate, amyl nitrite and sodium nitrite. Sodium nitrite works by forming methemoglobin which chelates CN. In fire victims that may already have carboxyhemoglobin in their bloodstream from CO poisoning, the metHb even further reduces the O2 carrying capacity of blood. So avoid sodium nitrite in cases of both CO and CN poisoning. If you have a case of both CO and CN poisoning and you don’t have access to hydroxocobalamin you can give the Sodium thiosulfate alone although slower and less effective than hydroxocobalamin.
Fluid Resuscitation in Burn and Inhalation Injuries
Key Concepts
- Over-resuscitation is just as harmful as under-resuscitation
- Ringer’s lactate is the preferred resuscitation fluid; children require maintenance (D5W+1/2NS) in addition to RL
- Formulas are just a starting point – titrate to urine output
- Avoid boluses whenever possible as they may increase the risk of compartment syndrome
- Avoid vasopressors whenever possible as vasoconstriction may devitalize burned tissue
The Parkland Formula is passé. Using the traditional Parkland formula of 4mL/kg tends to over-resuscitate most patients leading to complications such as abdominal compartment syndrome, orbital compartment syndrome, the need for escharotomies, impaired gas exchange and prolonged mechanical ventilation. Most experts now recommend a lower starting point. Check with your local burn center’s practice guideline as practice varies by jurisdiction. Avoid boluses and increase or decrease resuscitation fluid rate by 30% if hourly target not reached.
Modified Brooke/Parkland Formula is recommended as a starting point for fluid resuscitation for burns >15% BSA in children and >20% BSA in adults. Patients with inhalation injuries generally require more fluid resuscitation (closer to 4mL x %BSA x kg) however the extent of injury is impossible to quantify accurately, so instead, end-organ perfusion should be monitored carefully to help guide management. Aim for an hourly urine output of 30-50cc/hr in adults and 0.5-1cc/kg/hr in children. Children <30kg require maintenance fluids in addition to their resuscitation fluids. Children <1 year of age require the addition of Dextrose.
Maintaining Normothermia in Burn and Inhalation Injuries
Burn patients are at high risk of hypothermia as they have impaired thermoregulation. Ensure the room is warm and cover patients with warm dry blankets. Avoid wet dressings which can contribute to hypothermia. For transfer, the burns should be covered with dry sterile towels.
There is No Role for Prophylactic Antibiotics in Burn and Inhalation Injuries
There is no evidence to support the use of prophylactic antibiotics in burn and inhalation injuries patients. Administering antibiotics may increase the risk of resistant organisms and may increase the risk of fungal infections.
Indications for Consultation to a Burn Center
Burn Center Consultation Criteria
- Full thickness burns
- Partial thickness burns > 10%
- Burns to hands, face, genitalia, perineum, major joints
- Electrical (>600 V) or chemical burns
- Inhalation injury
- Special social, emotional or rehab needs
Key Take Home Points for Burn and Inhalation Injuries
- Think trauma and tox first; don’t get distracted by the burns
- Debride blisters, cover burns with antibiotic ointment and nonadherent dressings with reassessment within 72 hours
- For fires in an enclosed space or involving plastics, consider cyanide toxicity in addition to carbon monoxide poisoning and consider treating on speculation
- Use the Palmar Method for burns <15% and Lund & Browder for burns>15% rather than the Rule of 9s to estimate TBSA
- Use modified Brooke/Parkland to guide fluid management
- Fluid formulas are starting points only; titrate to urine output and end organ perfusion to avoid over- and under-resuscitation
Go to part 2 of this 2-part podcast on burn, inhalational, and electrical injuries
References
- American Burn Association. Burn incidence and treatment in the United States: 2011 fact sheet. http://www.ameriburn.org/resources_factsheet.php. Accessed February 10, 2011.
- Harshman J, Roy M, Cartotto R. Emergency Care of the Burn Patient Before the Burn Center: A Systematic Review and Meta-analysis. J Burn Care Res. 2019;40(2):166-188.
- Quinn K, Kriss S, Drapkin J, et al. Analgesic Efficacy of Intranasal Ketamine Versus Intranasal Fentanyl for Moderate to Severe Pain in Children: A Prospective, Randomized, Double-Blind Study. Pediatr Emerg Care. 2018.
- Cuttle L, Pearn J, McMillan JR, Kimble RM. A review of first aid treatments for burn injuries. Burns. 2009;35(6):768–775.
- Bartlett N, Yuan J, Holland AJ, et al. Optimal duration of cooling for an acute scald contact burn injury in a porcine model. J Burn Care Res. 2008;29(5):828–834.
- Avni T, Levcovich A, Ad-El DD, Leibovici L, Paul M. Prophylactic antibiotics for burns patients: systematic review and meta-analysis. BMJ. 2010;340:c241.
- Sargent RL. Management of blisters in the partial thickness burn: An integrative research review. J Burn Care Res 2006;27(1):66–81.
- Heggers JP, Ko F, Robson MC, et al. Evaluation of blister fluid. Plast Reconstr Surg 1980;65(6):798–804.
- Brandt CP, Yowler CJ, Fratianne RB. Burns with multiple trauma. Am Surg. 2002;68:240.
- Otterness K, Ahn C, Nusbaum J, Gupta N. Emergency Department Management of Smoke Inhalation Injury in Adults. Emerg Med Pract. 2018;20:1-2.
- Tolles J, Gupta N, Nusbaum J. Emergency Department Management of Patients with Thermal Burns. Emerg Med Pract. 2018:;20:1-24.
- Storm‐Versloot MN, Vos CG, Ubbink DT, Vermeulen H. Topical silver for preventing wound infection. Cochrane Database of Systematic Reviews 2010, Issue 3. Art. No.: CD006478.
FOAMed Resources
- AIME Infinity Airway Management eBook
- Scott Weingart. EMCrit RACC Podcast 219 – Critical Burn Patients in the ED/ICU – Part I with Dennis Djogovic. EMCrit Blog. Published on March 5, 2018. Accessed on May 21st 2019. Available at [https://emcrit.org/emcrit/critical-burn-patients-in-the-ed/ ].
- Modern Day Burn Resuscitation on EMDocs
Drs. Helman, Fish and Ivankovic have no conflicts of interest to declare









I was taught to avoid using antibiotic ointments containing neomycin (as many contain) . Many patients will have an adverse skin reaction to the neomycin and as such is best avoided . I tend to use simple petroleum jelly . Cheap and effective . Thoughts ?
As per discussions with Dr. Ivankovic: Neomycin tends to be more allergenic than most topical antibiotics so I avoid it in general. Polysporin fortunately does not contain neomycin but some people can develop a reaction to it or any topical preparation. With respect to reactions petrolatum alone is a safer option and certainly is cost-effective. I don’t know that there is great evidence that topical antibiotic ointment is better than just petrolatum on a clean burn but it is readily available in most departments so I think either one is a good choice for initial management in the ED.
I was wondering if the experts could expand a little on the evidence for the suggestion to debride blisters. (I’m sorry – I know you said you hated the topic)
My concern is that this is not a small ask. In my expedience, adding debridement in children changed them from a fast track type patient to a full procedural sedation, which adds not only risk to the patient, but significant problems with departmental flow. (We are even seeing more and more patients referred in from plastics clinics for debridement in the ED). I have never seen any evidence that this practice benefits, which makes me concerned that we are adding a lot of pain, ED inefficiency, and additional sedations for little to no benefit.
Of course, I have been wrong many times in my career, and would be happy to see evidence that I should change my practice.
Appreciate your thoughts, and the overall fantastic episode.
Thanks for your question Justin. To debride or not debride a burn blister has always been controversial but most burn experts currently recommend blisters be debrided. There has never been a randomized controlled trial to prove that debridement is better than leaving blisters intact and there may never be. Most of the recommendations are based on expert opinion and observational studies.
I completely agree that debridement typically requires procedural sedation and may be time consuming. If you have burn clinic follow up arranged within the next 48hrs I don’t think you will be faulted for leaving blisters intact particularly ones that are not impairing function or thick ones on the palms/soles (hands and feet need to be referred to a burn center anyway). Burn centers are very well equipped to sedate patients for proper debridement and dressing changes.
I do understand that inhalation injuries generally: require more fluid resuscitation and they are impossible to quantify. So in a patient with isolated inhalation injuries and in whom cyanide poisoning has been excluded what is a good starting point for resuscitation according to the modified Brooke/Parkland Formula? (especially when bronchoscopy is not immediately). Most referencing seems to be in inhalation burns WITH cutaneous burns as well, not just isolated inhalation burns.
Quiz vault released is slotted for June 18th. Thanks for your patience. Anton
There is no way to accurately quantify how
Much fluid extra to give. If you can monitor bp and urine output at 0.5 cc kg hr gou can add 20 to 30 percent more fluid as a guide. This is true for adults and children. The real issue at play is what to do when the oxygenation and ventilation start to deteriorate and you still beed fluid for the large cutaneous burn! This requires critical care expertise beyobd that which most emergency rooms would deal with
Not clear about pain relief options .
Intranasal will be great for young -20-25 kg but older children and adults say 25kg -100kg what is recommended for acute pain interim between dressing changes and during dressing changes .