In this first installment of this Episode, Point of Care Ultrasound Pearls, Pitfalls & Controversies we have a panel of POCUS gurus, Dr. Greg Hall, Dr. Jordan Chenkin, Dr. Paul Hannam & Dr. Jason Fischer.They review the basic criteria for commonly used, practical Point of Care Ultrasound indications at the bedside and then dive into heated debate about specific pearls and pitfalls in Point of Care Ultrasound assessment of the patient with undifferentiated shortness of breath, undifferentiated shock, cardiac arrest and swollen leg. They discuss how best to interpret the massive body of literature for POCUS and when we can hang our hats on our Point of Care Ultrasound findings.
Our panel of experts answer questions such as: How does 2-point compression Point of Care Ultrasound of the leg compare to radiology department ultrasound for DVT? How does POCUS for pneumothorax compare to CXR and CT? In what situations does cardiac standstill on POCUS not suggest futile resuscitation? Can evaluation of RV function on Point of Care Ultrasound help us decide whether or not to thrombolyse a patient with submassive pulmonary embolism? How can POCUS help in diagnosing CHF? What is the best anatomical approach for pericardiocentesis? How can Point of Care Ultrasound help us in the crashing pediatric patient? and many more……
Written Summary and blog post by Lucas Chartier, edited by Anton Helman Oct 2011
Cite this podcast as: Hall, G, Chenkin, J, Hannam, P, Fischer, J, Helman, A. Part 1: Point of Care Ultrasound Pearls, Pitfalls and Controversies. Emergency Medicine Cases. October, 2011. https://emergencymedicinecases.com/episode-18-part-1-point-of-care-ultrasound-pearls-pitfalls-controversies/. Accessed [date].
Point of Care Ultrasound for Pericardial effusion
- Technique
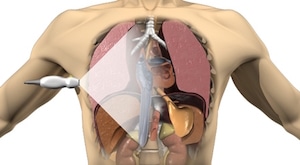
- subxiphoid view – 96-98% sensitivity and easiest to learn: focus on the area where the inter-ventricular wall connects with the apex of the heart and sweep anteriorly and posteriorly (where blood most often pools)
- Pitfalls
- epicardial fat pad may appear like an effusion, but is more prominent anteriorly,
- clotted blood may be more dense and be missed, and
- presence of effusion does NOT rule in or out cardiac tamponade, which is a clinical diagnosis
- Ultrasound-guided pericardiocentesis
- insert needle at the apex of the heart (as opposed to the trans-diaphragmatic approach) where there’s the biggest pocket of fluid is and where there’s fewer obstacles between the skin and the effusion
Point of Care Ultrasound for Pneumothorax
- Sensitivity (98-99%) much better than CXR, especially in supine trauma patient where pleural air is travelling anteriorly, and faster to obtain
- Technique: High-frequency linear probe placed on the most anterior portion of the chest in a supine patient, in the mid-clavicular line, and look for:
- Lung sliding: i.e. ‘ants marching on a string’, as the visceral and parietal pleura move relative to each other; if air is between the pleura, the ultrasound waves get scattered and you don’t see sliding
- Comet tails: bright white beams of light going deep in the screen, caused by water droplets in the interlobular septae in the visceral pleura, and absent in pneumothorax (PTX)
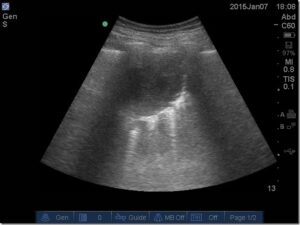
- Lung point: used as confirmation tool, and located where visceral and parietal pleura are separating at the origin of the PTX, found by sliding the US probe laterally until the separation point is found – very specific for PTX
- PNX Size Determination: small if no lung sliding at anterior axillary line, moderate if no lung sliding at mid-axillary line, large if no lung sliding at posterior axillary line – 95% agreement between ultrasound (US) and CT scan
- False positives: bullous disease in COPD, pulmonary fibrosis, pulmonary contusions and mainstem intubation (will have no lung sliding but may have comet tails)
For a PV card on focused lung assessment using POCUS on the ALiEM blog here.
Point of Care Ultrasound for Undifferentiated Shock
- Causes
- hypovolemic (bleed, dehydration)
- distributive (sepsis, anaphylactic)
- cardiogenic (MI, cardio-myopathy, valvular)
- obstructive (cardiac tamponade, pneumothorax, pulmonary embolus) – POCUS may help!
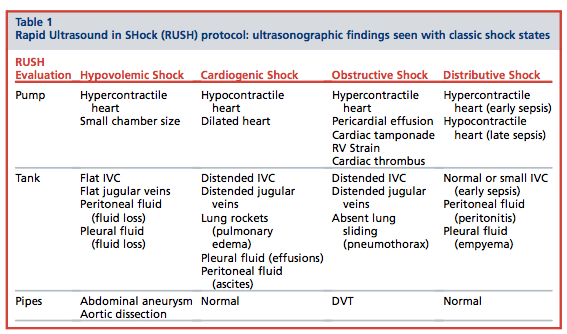
RUSH (Rapid Ultrasound in SHock) protocol
- To be used in undifferentiated shock, in a step-by-step algorithm to guide diagnosis and early management
- PUMP (i.e. the heart): Look at the heart for pericardial effusion (cardiac tamponade), contractility of the left ventricle (ischemia), and relative size of right and left ventricles (right heart strain in PE)
- TANK (i.e. intravascular volume assessment): IVC assessment (size, collapsibility) and ‘tank compromise’, i.e. PTX
- PIPES (i.e. major arteries and veins): Assessment for AAA or dissection flap, and DVT in legs Mnemonic to remember the order: HIMAP – Heart, IVC, Morrison’s pouch and FAST exam, Aorta, PTX
From Perera et al. The RUSH Exam: Rapid Ultrasound in Shock in the Evaluation of the Critically Ill. Ultrasound Clinics N Am 28 (2010) 29–56.
Full PDF: https://www.dtod.ne.jp/ohtablog/images/article10_pdf_003.pdf
Point of Care Ultrasound for Pulmonary Embolism
Ultrasound is neither sensitive nor specific for PE but may help in 1. thrombolysis and 2. disposition decisions
- Submassive PE & thrombolysis: While there is clear evidence for benefit of thrombolysis in massive PE, in submassive PE where the patient is NOT in shock, but has evidence of right heart dysfunction on US or ECG, or who has positive troponin or BNP biomarkers – controversy exists regarding thrombolysis given that bleeding risks may outweigh potential benefits. In deciding which patients with submassive PE should receive thrombolysis, some experts suggest lysis if severe right-heart strain on US, which may indicate a pre-shock state.
For discussion on detection and treatment of submassive PE see Episode 61
- Dispostion: Compare right and left ventricular sizes in apical view (right ventricle is on the left in the image below), and consider it in right-heart strain – if right heart strain present, consider inpatient therapy even if patient appears well
Hypodynamic vs. hyperdynamic left ventricle
Hyperdynamic, i.e. small ventricle with >70% (on gestalt) change in diameter of ventricle in systole (or if the walls touch) – 94% specific for failure in non-traumatic shock patient
ICV diameter (i.e. intravascular volume assessment)
- In long axis (longitudinal plane) view, assess anterior-posterior diameter of IVC:
- Size: if <1cm, patient likely volume depleted; if >2cm, unlikely volume depleted
- Variability: If no variation of size with respiration, likely not hypovolemic; if IVC collapses with respiration, likely hypovolemic
- Intubated patient: IVC will increase with respiration due to positive pressure ventilation (as opposed to usual negative pressure)
- Pediatric hydration status: Compare IVC to aorta; normal ratio 1.2:1, and can help to guide fluid therapy
- PEARL from the experts: use US for intra-osseus needle placement confirmation: high-frequency probe placed next to IO to see flow beneath cortex in Doppler mode
Role of Point of Care Ultrasound in Cardiac Arrest Resuscitation
- US may be used as an adjunct to stop resuscitative efforts, but there’s no absolute criteria
- Early phase of cardiac arrest: US may help with the H’s and T’s, i.e. tamponade, PTX, AAA, PE and volume resuscitation
- Later phases: assess for cardiac standstill, i.e. patient very unlikely to survive code (except in pediatric hypoxic arrest and hypothermic arrest), and may be useful for family members to see that the heart has stopped beating – survival is <<1% (likely close to 0%)
- Do not interrupt chest compressions to use US! Rather, use US at the 2min intervals when checking for pulse
Can Point of Care Ultrasound help Confirmation of ETT placement?
Quantitative capnography still the gold standard, but if lung sliding is only seen unilaterally on the right, consider right mainstem bronchus intubation and pull on the ETT until lung sliding is seen bilaterally
Point of Care Ultrasound for Deep vein thrombosis (DVT)
- 2-point compression testing is reliable in select patients (no chronic or recurrent DVTs, no obese patients)
- Most useful in situations where you are considering giving LMWH ‘on spec’ and arranging outpatient radiology department ultrasound. If emergency bedside ultrasound is negative, consider not treating with LMWH until the confirmatory US is obtained.
- May also be useful in undifferentiated shock patient to help rule in pulmonary embolism.
Check out the PV Card on ALiEM for a summary of how to do POCUS for DVT.
Interpreting the emergency ultrasound literature
- There is a huge body of literature for point of care ultrasound, which can be overwhelming to interpret for the practicing clinician, and with results that appear very impressive at first glance. However, these studies must be interpreted with ‘a grain of salt’ as most have at least one of the following limitations:
- Generalizability: clinician-ultrasonographers in studies are often few and very experienced, which doesn’t mean that most clinicians would obtain the same levels of sensitivity and specificity
- Biases: on top of the inherent biases of the authors themselves, there is ‘destiny bias’ – if seeing cardiac standstill on the US influences your decision to stop the resuscitative efforts, the study results will obviously be influenced by this
- Convenience sampling: young, slim and healthy volunteers (or patients) are often chosen by ‘convenience’ because they are much easier to scan than the real life patients who are older and bigger
- Publishing bias: negative studies probably don’t get published as much
- Outcomes: studies often compare imaging outcomes (PTX on CXR and US vs. CT scan), but not clinically- relevant outcomes (eg, are those occult PTX found by US clinically significant?)
- Ethics: for some indication for which US is now the standard of care (eg, FAST), it is not ethical to randomize patients to FAST vs. no-FAST, and therefore we might never get grade I evidence for certain modalities that we already use
For more on Point of Care Ultrasound on EM Cases:
Episode 18 Part 2: More Point of Care Ultrasound
Best Case Ever 6 Can Point of Care Ultrasound Save Lives?
POCUS Cases videos
Key References
Perera et al. The RUSH Exam: Rapid Ultrasound in Shock in the Evaluation of the Critically Ill. Emerg Med Clin N Am 28 (2010) 29–56.
Arntfield RT, Millington SJ. Point of care cardiac ultrasound applications in the emergency department and intensive care unit–a review. Curr Cardiol Rev. 2012;8(2):98-108.
Akilli B, Bayir A et al. Inferior vena cava diameter as a marker of early hemorrhagic shock: a comparative study. Ulus Travma Acil Cerrahi Derg 2010;16(2):113-8.
Chou HC, Chong KM, Sim SS, et al. Real-time ultrasonography for confirmation of endotracheal tube placement during cardiopulmonary resuscitation. Resuscitation. 2013 Dec;84(12): 1708-12.
Fox JC, Bertoglio KC. Emergency Physician Performed Ultrasound for DVT Evaluation. Thrombosis. 2011;2011:938709.
Dr. Fischer, Dr. Hannam, Dr. Chenkin and Dr. Hall have no conflicts of interest to declare.





Leave A Comment