Current estimates of the prevalence of obesity are that a quarter of adult Canadians and one third of Americans are considered obese with approximately 3% being morbidly obese. With the proportion of patients with a BMI>30 growing every year, you’re likely to manage at least one obese patient on every ED shift. Obese patients are at high risk of developing a host of medical complications including diabetes, hypertension, coronary artery disease, peripheral vascular disease, biliary disease, sleep apnea, cardiomyopathy, pulmonary embolism and depression, and are less likely compared to non-obese adults to receive timely care in the ED.
Not only are these patients at higher risk for morbidity and mortality, but obesity emergency management is complicated by the patient’s altered cardiopulmonary physiology and drug metabolism. This can make their acute management much more challenging and dangerous. To help us gain a deeper understanding of the challenges of managing obese patients and elucidate a number of important differences as well as practical approaches to obesity emergency management, we welcome Dr. Andrew Sloas, the founder and creator of the fantastic pediatric EM podcast PEM ED, Dr. Richard Levitan, a world-famous airway management educator and innovator and Dr. David Barbic a prominent Canadian researcher in obesity in emergency medicine from University of British Columbia….
Podcast: Play in new window | Download (Duration: 1:05:33 — 60.1MB)
Subscribe: Apple Podcasts
Written Summary and blog post prepared by Dr. Michael Kilian, edited by Dr. Anton Helman, Sept 2015
Cite this podcast as: Sloas, A, Levitan, R, Barbic, D, Helman, A. Obesity Emergency Management. Emergency Medicine Cases. September, 2015. https://emergencymedicinecases.com/obesity-emergency-management/. Accessed [date].
Obese patients are not just large adults!
Vital Signs in Obesity Emergency Management
Blood pressure readings can be falsely reassuring in obese patients as the cuff often overestimates BP. A ‘borderline’ BP could represent a shock state in an obese adult. If you recognize that a blood pressure within the normal range does not rule out shock in an obese patient who appears unwell, you are more likely to begin early resuscitation and initiate appropriate treatment. In order to obtain a more accurate reading, consider placing an early arterial line to obtain and trend accurate BP readings over time.
The Shock Index can be a helpful tool in making a diagnosis of occult shock in obese and non-obese patients. The calculation requires accurate readings for prognostication.
Shock Index = HR/SBP
Any number > 1 suggests occult shock
Shock index calculator interpretation and references at MDCalc
ECG Alterations in Obesity Emergency Management
The ECG in obese patients also differs from the average adult. The ECG of an obese patient is more likely to show:
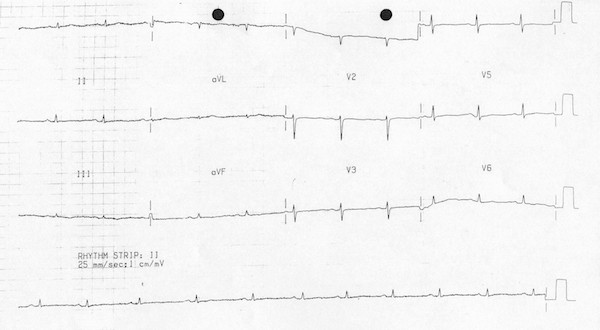
1. Low voltages – due to the size of their chest wall; note that it is important to rule out a pericardial effusion when you see low voltages, before attributing these findings to adipose tissue alone
2. Longer QT intervals – rarely >500ms as a result of obesity alone
3. Signs of Left Ventricular Hypertrophy (LVH) – consider an echocardiogram to rule out obesity-associated cardiomyopathy
Low Voltage ECG. Courtesy of Lifeinthefastlane.com
Important Pathophysiologic Considerations in Obesity Emergency Management
- Decreased respiratory reserve is secondary to diminished total lung capacity and functional residual capacity. The decreased reserve compromises an obese patient’s ability to tolerate respiratory insults such as pneumonia
- Increased airway pressures are a result of increased airway resistance (heavier chest walls, increased abdominal girth, atelactatic lung bases). The increased pressures lead to:
- Smaller oxygen reserves at baseline
- Increased work of breathing
- Shorter time to desaturation during induction and a shorter Safe Apnea Time
- Higher incidence of hypoxemia and hypercapnia at baseline
- Higher risk of aspiration pneumonitis
- More difficult to ventilate with BMV
Dr. Levitan created a helpful mnemonic for all of the factors that need to be considered in planning and executing a safe and successful intubation for critically ill obese patients:
V.A.P.O.R.S
Ventilation
Acidosis
Pressures (BP, peak pressures, plateau pressures etc)
Oxygenation
Regurgitation
Shock Index (see above)
For details on Dr. Levitan’s VAPORS approach visit Mayo EM Blog
Ventilation and Induction in Obesity Emergency Management
Applying what we know about the pathophysiological differences in obese patients’ airway and their ability to tolerate acute insults, the following mnemonic outlines a practical approach to the airway of the obese patient (care of edtcc.com):
B.I.G.R.A.M.P
BUY TIME: Given the decreased respiratory reserve and higher degrees of hypoxemia, increase the FiO2 and recruit as much lung space as possible.
- Provide 100% FiO2
- Insert nasal trumpets
- Use non-invasive positive pressure ventilation to recruit alveoli
- Provide a two handed bilateral jaw thrust
- Optimize medical therapy: Resuscitate before you intubate! This may require large, rapid fluid boluses or initiation of vasopressors before induction via a peripheral IV
- If all else fails, a supraglottic airway can provide a useful bridge to a definitive airway
INDICATION FOR INTUBATION: Consider whether you really need to intubate now and if you have time to optimize the patient first.
GET HELP: The obese patient presents an anticipated challenging airway. Therefore, the most experienced physician should be the first to attempt intubation. Consider calling your colleagues from anaesthesia, ICU or ENT.
RAMP: Build a big ramp behind the patient’s head and torso to achieve an ear-to-sternal-notch configuration with towels or commercially available products. Then position the patient in reverse Trendelenburg to take the weight of the panus off the chest.
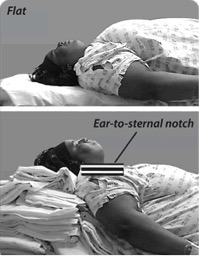
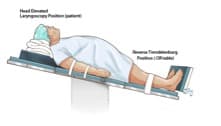
For more on positioning the obese patient for airway management visit Airway eLearning
Dr. Levitan’s lecture on Head Positioning:
https://www.youtube.com/watch?v=-2wXE56N8kE
APNOEIC OXYGENATION: Use nasal cannulas at 15L underneath the facemask or bag-valve-mask to maintain diffusion of oxygen and help blow open the oropharynx
see Episode 54 – Pre-oxygenation and Delayed Sequence Intubation for details on apneic oxygenation
MINIMAL DRUGS: consider lidocaine spray and/or small doses of ketamine
PRE-OXYGENATE WITH NIV: This will help improve Safe Apnea Time in patients with decreased respiratory reserve
PARALYSIS – Dr. Levitan recommends against paralysis in most critically ill obese patients. Once paralyzed you may encounter a “can’t oxygenate, can’t ventilate” situation.
PLAN FOR FAILURE
Make sure to have at least two functioning intravenous access ports before initiating induction. This may require the use of ultrasound to place a large bore IV or placement of an IO. For intra-osseous access, use the largest bore needle (Yellow 45mm needle in EasyIO kits) for obese patients and consider humeral or sternal IO placement if IV access cannot be readily obtained and you encounter too much adipose tissue at the pre-tibial location. A femoral central line can be quickly placed with the patient in frog-legged position and an assistant displacing the patient’s panus. Our experts recommend against placing neck central lines in massively obese patients because of the ill effects of placing obese patients in Trendelenburg position and because of the theoretical increased risk of complications.
Have a cricothyrotomy kit at the bedside for all anticipated challenging airways in obese patients. For cricothyrotomy in obesity emergency management, Dr. Levitan recommends first identifying the midline using the laryngeal handshake technique or ‘rocking the rhomboid‘ and cutting a large vertical skin incision rather than first attempting to identify the cricothyroid membrane through the adipose tissue.
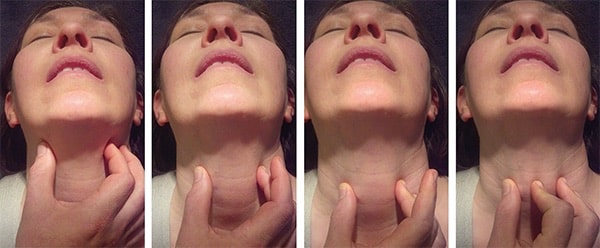
POST INTUBATION CARE: The ventilator settings will need to provide higher PEEP and plateau pressures than the average adult. Continuing the ramped and reverse Trendelenburg position in post-intubation care can help decrease the pressures required.
Pharmacologic Adjustments in Obesity Emergency Management
Consulting with a pharmacist will help you dose medications appropriately based on their pharmacodynamics.
Lipophilic drugs (eg. Propofol) need to be dosed based on total body weight. Therefore these doses will be much higher than in average adults.
Hydrophilic drugs (eg. Ketamine) are dosed based on ideal body weight.
Antibiotics also have different dosing profiles based on their class. Vancomycin loading doses are 25-30mg/kg of total body weight. Beta-lactams (eg. Pipiracillin-tazobactam) doses are based on ideal body weight with an additional conversion factor that your pharmacist can help you with.
Trauma & Obesity Emergency Management
Obese patients have a higher risk for sustaining severe trauma. Compared to the average-sized adults with a similar injury severity score (ISS), they have higher rates of morbidity and mortality. Studies have shown that obese patients are less likely to wear their seat belts and are more likely to sustain chest injuries than abdominal injuries.
When an obese patient arrives in your trauma bay, you should be aware of important limitations in your assessment and workup of these patients. Firstly, the blood pressure cuff will be unreliable as mentioned earlier. Therefore you may be more likely to miss shock or under-resuscitate your obese trauma patient. Your imaging modalities will also be less reliable. The FAST scan may be indeterminate or falsely negative given the depth of penetration required to visualize Morrison’s pouch. The chest x-ray will be under-penetrated. Finally, the CT images will be more difficult for the radiologist to interpret and as a result, injuries are more often missed.
Unfortunately, some patients may be too heavy to have a CT scan performed. Different CT scanners have varying weight cut-offs but most have a weight limit in the range of 350-450lbs. In order to image heavier patients, a bariatric CT scanner is required. Speak to your radiologists to develop a protocol for transferring massively obese patients to the closest bariatric CT scanner.
When it comes to placing a chest tube in an obese trauma patient, similar to the adjustments necessary for a cricothyrotomy, our experts suggests a larger skin incision to help navigate the palpation through the deep adipose tissue to help locate the intercostal space.
Dr. Claire Atzema’s Best Case Ever involving the management of an obese patient in atrial fibrillation
Key References
Heffner AC, Swords DS, Neale MN, Jones AE. Incidence and factors associated with cardiac arrest complicating emergency airway management. Resuscitation. 2013;84(11):1500-4. Full pdf
Dargin J, Medzon R. Emergency department management of the airway in obese adults. Ann Emerg Med. 2010;56(2):95-104. Full pdf
Collins JS, Lemmens HJ, Brodsky JB, Brock-utne JG, Levitan RM. Laryngoscopy and morbid obesity: a comparison of the “sniff” and “ramped” positions. Obes Surg. 2004;14(9):1171-5. Abstact
Mechanick JI, Youdim A, Jones DB, et al. Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient–2013 update: cosponsored by American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery. Obesity (Silver Spring). 2013;21 Suppl 1:S1-27. Full pdf
Dr. Helman, Dr. Sloas, Dr. Burbic & Dr. Levitan have no conflicts of interest to declare




[…] Helman welcomes Rich Levitan, Andy Sloas and David Barbic to discuss the management of the critically ill obese patient. […]