In this EM Cases Episode 131 PEA Arrest, PseudoPEA and PREM with Rob Simard of POCUS Cases fame and the co-author of The POCUS Pulse Check paper and Scott Weingart, we go beyond ACLS and guide you through the complex world of Pulseless Electrical Activity (PEA). We discuss the notion that the palpation technique is poor at determining whether or not a patient has a pulse, that the POCUS pulse is more accurate and as rapid, compared to the palpation technique, at determining whether or not a patient has a pulse, the difference between true PEA arrest, PseudoPEA and PREM, why epinephrine may be harmful in PEA, Weingart’s chain of survival approach from PEA arrest to Return of Spontaneous Circulation (ROSC), four tools to help differentiate true PEA arrest from PseudoPEA or ROSC, how to prevent long pauses in chest compressions using POCUS, EM Cases PEA arrest and PseudoPEA suggested dynamic algorithm, vasopressor choices in PseudoPEA, whether the “QRS wide vs narrow width” approach to PEA arrest underlying cause is useful or not and much more…
Podcast: Play in new window | Download (Duration: 55:09 — 50.6MB)
Subscribe: Apple Podcasts
Podcast production, sound design & editing by Anton Helman
Written Summary and blog post by Anton Helman October, 2019
Cite this podcast as: Helman, A. Simard, R. Weingart, S. PEA Arrest, PseudoPEA and PREM. Emergency Medicine Cases. October, 2019. https://emergencymedicinecases.com/pea-arrest-pseudopea-prem. Accessed [date]
The palpation technique is poor at determining whether or not a patient has a pulse
In a study assessing the diagnostic accuracy of first responders of detecting a manual pulse in patient with and without a true pulse, the sensitivity for pulselessness approached 90%, however the specificity was only 55%. Only 15% of participants could accurately assess for the presence of a pulse within 10 seconds and only 2% identified pulselessness correctly within 10 seconds.
A study of EM and ICU physicians and nurses attempting manual pulse determination in healthy subjects demonstrated that 43% of participants required more than 5 seconds to detect the pulse.
An observational study of 105 healthcare providers showed that only 38% correctly identified a pulse and only 9% correctly identified pulselessness within 10 seconds by palpation method.
“Humans are reliably unreliable at finding pulses with their fingers” – Scott Weingart
The POCUS pulse is more accurate and as rapid compared to the palpation technique at determining whether or not a patient has a pulse
A 2019 RCT of 111 health care providers with 15 minutes of US training in detecting carotid pulses looked at time to carotid pulse detection and rates of prolonged pulse checks (>5 or 10 seconds), showed no significant differences between POCUS pulse check and manual pulse check in the rates of prolonged pulse checks of greater than 5 or 10 seconds. First attempt at detection of a pulse was more successful in the POCUS group (99.1% vs 85.6%).
In a case series comparing POCUS pulse checks with manual pulse checks POCUS pulse checks were consistently performed in < 5 seconds and clearly determinate, even when palpation yields indeterminate results.
Update 2020 A study of patients looked at accuracy of POCUS pulse check. They compiled a library of 10-second clips of the common carotid artery at high-, medium- and low-SBPs and pulseless clips while on bypass. They then showed these clips to critical care physicians and asked them to answer whether or not there was a pulse within 10 seconds, using the arterial line trace as the gold standard. Twenty-three patients had all four videos collected. Overall sensitivity was 91% and specificity 90%. Sensitivity was highest in the high-SBP group (96%) and lowest in the low-SBP group (84%). https://www.resuscitationjournal.com/article/S0300-9572(20)30500-1/fulltext
The difference between true PEA arrest, PseudoPEA and PREM
PseudoPEA was first described in 1992 in an article that describes the use of arterial lines demonstrating an arterial waveform in some patients presumed to be in PEA arrest.
- Both true PEA and PseudoPEA have organized activity on the monitor and
- Inability to detect a pulse by palpation
True PEA is truly a pulseless state and there is no cardiac output
In Pseudo PEA a pulse is not palpable by the manual technique, however there is cardiac output that we are not able to detect by the palpation technique, but are able to detect with a POCUS pulse check, arterial line, ETCO2 and oxygen saturation waveform.
PseudoPEA is a profound shock state, not cardiac arrest.
Because of some ambiguity around the definition of PseudoPEA, another lexicon has been suggested:
PRES = Pulseless with a Rhythm with Echocardiographic Standstill = true PEA
PREM = Pulseless with a Rhythm with Echocardiographic Motion = PseudoPEA
Epinephrine may be harmful in PEA arrest and PseudoPEA
The beta-adrenergic effects of epinephrine (increased cardiac rate, contractility, and automaticity) are potentially harmful as they may lead to dysrhythmias and increased myocardial oxygen demand and ischemia.
Overall, the NNT for epinephrine in cardiac arrest to achieve ROSC prior to hospital arrival is 7, however the number needed to harm for poor long term neurologic outcome is 83. In a study of cardiac arrest patients who achieved ROSC comparing epinephrine to no epinephrine, there were significantly lower rates of neurologically intact survival in the patients who had received epinephrine, with higher doses of epinephrine associated with lower odds of neurologically intact outcome, in a dose-dependent fashion. The PARAMEDIC-2 trial, showed improved ROSC and, for the first time in history, improved 30 day survival, but at the cost of worse long term neurologic outcomes.
Many experts are currently recommending no more than 3 doses of epinephrine 1mg in cardiac arrest. From an ED perspective, usually EMS have given 1 or 2 or 3 doses in the field already, so consideration for only 1 or no doses of epinephrine in the ED should be entertained.
In patients with PseudoPEA, the potential deleterious effects of epinephrine are likely exaggerated.
Learn more about epinephrine in cardiac arrest in EM Cases Journal Jam 14
Weingart Chain of Survival Approach from PEA arrest to ROSC
This is a useful way of thinking about where a patient is on the spectrum from full true PEA cardiac arrest to return of spontaneous circulation with persistent perfusion of vital organs, in order to guide management.
- Rhythm capable of perfusion
- Rhythm capable of causing cardiac contraction
- Cardiac contraction sufficient to generate a pulse
- Pulse generates a sufficient BP to perfuse vital organs

From EMcrit https://emcrit.org/emcrit/pea-is-stupid/
4 tools to help differentiate true PEA arrest from PseudoPEA or ROSC
- POCUS – is there cardiac contractility? is there a femoral or carotid pulsation?
- Arterial line – shows persistent DBP>30-40 (best option)
- Oxygen saturation waveform – from a finger probe shows a persistent waveform
- End-tidal CO2 – persistent elevations >30-40
Use of POCUS may prolong pauses in chest compressions if used indiscriminately and has not been shown to definitively improve neurologically intact outcomes in cardiac arrest
Several observational studies have shown that use of POCUS during cardiac arrest prolongs pauses in chest compressions, however a recent study showed that with minimal training POCUS pulse checks were more accurate than manual pulse checks and completed accurately within 5 seconds.
The REASON Trial was a multicenter prospective observational study of 793 patients with out-of-hospital cardiac arrest comparing arrests run with POCUS performed at the beginning and end of the arrest and without. While survival to hospital admission and hospital discharged looked promising for the POCUS group, it is unclear whether POCUS improved neurologically intact long term survival.
How to prevent long pauses in chest compressions using POCUS
- Generate the image during chest compressions
- Team member counts down from 10 before pause in chest compressions while POCUS team member prepares to interpret and record image
- Record a video for 4-5 seconds during the chest compression pause and watch it after chest compressions have resumed if further interpretation is required
Which cardiac POCUS view is best in cardiac arrest?
A systematic review and meta-analysis of 11 studies with a total of 777 PEA patients found that the use of a subxiphoid view alone was not associated with improved rates of ROSC in PEA arrest, while the use of other cardiac POCUS views was associated with improved rates of ROSC. One approach, based on opinion only, is to use a subxiphoid view for the initial assessment of cardiac contractility and utilize other views later in the resuscitation to rule out causes of PEA.
EM Cases PEA arrest and PseudoPEA suggested dynamic algorithm
Note that this algorithm is not evidence-based, deviates from published guidelines, assumes a team of at least 4 people, and that PEA management is a dynamic process depending on local resources and patient clinical characteristics. EMS and collateral history may help guide this dynamic process.
Preparation before the PEA arrest patient arrives in the ED
- Draw up “push dose” epinephrine and prepare a norepinephrine infusion to be started as the patient arrives running in the background at 10-50 micrograms/min.
- Turn on/gel up the POCUS machine and call for a dedicated, skilled user if available
- Airway gear to the bedside including bougie, LMA and cric kit and call for a dedicated, skilled airway person if available
- Oxygen saturation, ETCO2, arterial line gear at the bedside and call for a dedicated person to place the arterial line if available
- Call for two dedicated people to perform chest compressions, preferably with in-line feedback or a metronome set to 110 bpm
- Announce your plan to your team
This algorithm assumes ACLS algorithm as a default. For teams <4 people, priorities are high quality chest compressions, IV access, POCUS pulse checks, ventilation and oxygenation.
First pause in chest compressions: perform a POCUS pulse check at the femoral (or carotid) artery (maximum 10 seconds, usually takes 5 seconds)
If no POCUS pulse seen, resume chest compressions, administer epinephrine 1 amp, assess ETCO2 (as per ACLS guidelines) and/or place arterial line and set up for cardiac POCUS for the second rhythm/pulse check, draw and send STAT electrolytes from a blood gas.
If POCUS pulse seen, treat as profound shock state: do not resume chest compressions, hold epinephrine 1 amp, assume cardiac contractility and assess for brain and heart perfusion by persistent presence of oxygen saturation waveform and/or ETCO2>40 and/or arterial line DBP>40 and/or cuff MAP ≥50-60; maintain or start norepinephrine 10-50 micrograms via well running antecubital peripheral IV and titrate to MAP of ≥60, correct hypoxemia and hypovolemia and search for causes of PEA using cardiac, lung and abdominal POCUS, ECG, electrolytes from a blood gas and EMS/collateral history.
Second pause in chest compressions: perform a cardiac POCUS (subxiphoid or alternate view) by generating an image at least 10 seconds prior to pausing chest compressions and as chest compressions are stopped hit the video record button, attempt interpretation of the image in 5-10 seconds maximum, resume CPR and, if need be, watch the video clip for further interpretation looking for: vigorous cardiac contractility (not only valve motion), and clues to anatomical causes of PEA to be interpreted appropriately in the specific clinical setting – collapsed RV (cardiac tamponade or tension pneumothorax), enlarged RV with septal bowing (pulmonary embolism), severe poor LV function (MI).
If vigorous cardiac activity on POCUS but no POCUS pulse (based on the first POCUS pulse check), this is most likely due to profound hypovolemia. There are 2 options:
- Resume CPR, administer 1 amp epinephrine if <3 have been administered, while aggressively searching for and reversing causes as per ACLS guidelines (with focus on causes of profound hypovolemia), or
- Treat as profound shock state: pause chest compressions and repeat the POCUS pulse check to see if a pulse has been generated in the interim, assess for other signs of ROSC (oxygen saturation waveform, ETCO2 and DBP on arterial line) and administer or titrate vasopressor (see vasopressor choices below).
Note that animal studies have suggested poor cardiac output with chest compressions performed during cardiac contractility although synchronized mechanical chest compressions studies have suggested improved cardiac output with chest compressions during cardiac contractility.
Third and fourth pauses in chest compressions: (ideally using 2 ultrasound machines – one for POCUS pulse and other searching for PEA causes) perform a lung POCUS during one pause in compressions while assessing for manual pulse (or POCUS pulse with a second machine) and signs of end-organ perfusion, and an abdominal POCUS during another pause in compressions, the order depending on the clinical scenario, looking for clues to anatomical causes of PEA – tension pneumothorax (collapsed RV, lack of lung sliding, lack of power slide, absence of normal comet tail or reverberation artifacts, presence of a “lung point” or “transition point”), ruptured AAA, severe hypovolemia (flat IVC, free fluid).
Vasopressor options in PseudoPEA
3 vasopressor options:
- Norepineprhine infusion: If you have time before the patient arrives get your norepinephrine drip ready so that you can start it as the patient arrives or as needed. Our experts recommend starting starting either at 10 micrograms and titrating up to 20-30, or starting at 50 micrograms and titrating down to 20-30 as needed.
- Epinephrine “push dose pressor”: Take a 10 ml syringe with 9 ml of normal saline. Into this syringe, draw up 1 ml of epinephrine from the cardiac amp (amp contains Epinephrine 100 mcg/ml). Now you have 10 mls of Epinephrine 10 mcg/ml. Administer 0.5-2 ml every 1-5 minutes (5-20 mcg).
- Vasopressin: Give vasopressin 20IU as a bridge to getting your norepinephrine drip infusing.
QRS Width Approach to PEA Arrest Underlying Cause: Useful or not?
In an effort to improve recall of the “5 Hs and Ts” underlying causes of PEA arrest, Littman in 2014 published an approach to PEA, dividing up patients into those with a wide QRS complex and those with a narrow QRS complex with their most likely causes and using POCUS to help differentiate the anatomical underlying causes of the PEA arrest. The idea was that narrow-complex PEA is generally due to mechanical problems caused by RV inflow or outflow obstruction and wide-complex PEA is typically due to metabolic problems. MI can have either wide or narrow complex QRS.
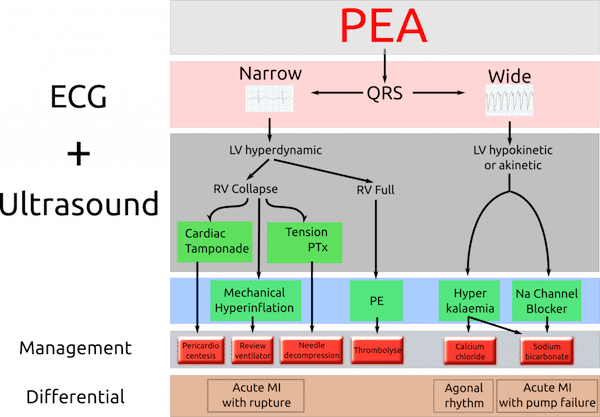
From Adelaide Emergency Physicians Education Resource
However in 2016 Bergman challenged the Wide vs Narrow QRS Complex approach as an accurate way of determining the underlying cause in a prospective study of 51 patients with in-hospital cardiac arrest and PEA. It suggsted that there were no unique ECG patterns associated with any particular underlying cause of PEA.
Evidence debunking the narrow vs wide complex approach to PEA arrest by Rory Speigel on EMCrit
Our experts disagree on the usefulness of this approach. On the one hand this approach may help the clinician recall the most important causes of PEA more readily that the “5 Hs and Ts” list. On the other hand having a poster on the resuscitation bay wall with the “5 Hs and Ts” or laminated card for EMS personnel may be a better way of recalling the underlying causes of PEA arrest.
Take home points for PEA Arrest, PseudoPEA and PREM
- Just because you cannot feel a pulse with your fingers does not mean the patient is pulseless.
- You can distinguish between PseudoPEA and true PEA with the aid of POCUS, an arterial line, oxygen saturation waveform and end-tidal CO2.
- The distinction between true PEA and PseudoPEA is likely to change your management from usual cardiac arrest management to profound shock management.
- POCUS can lead to delays in chest compressions and prolonged pulse checks if used indiscriminately so make sure that you have the logistics practiced so that you are spending no longer than 5-10 seconds without chest compressions in true PEA.
- Before the patient arrives consider preparing a norepinephrine infusion at 10-50 micrograms per minute and start it as the patient arrives.
- Ask yourself 4 questions to guide management: Do they have a perfusable rhythm? Do they have cardiac contractility? Do they have a pulse from that contractility? Do they have a sufficient BP to perfuse vital organs?
- To distinguish true PEA from pseudoPEA use at the very least an O2 sat waveform, end tidal CO2, POCUS either on the heart in the first pause from chest compressions or on the femoral and an arterial line if you have the person power, necessary gear and skill.
- If you determine that PseudoPEA is present or if the patient has already received 3 doses of epinephrine in the field, rather than administering 1mg IV epinephrine, give volume and a titratable pressor: norepinephrine, vasopressin or push dose epinephrine.
- Use the EMS/collateral history, POCUS and electrolytes off the blood gas to help you with the differential diagnosis. While the wide vs narrow QRS complex approach has been debunked in one study, it may nonetheless be useful as a memory aid.
References for PEA Arrest, PseudoPEA and PREM
Manual and POCUS Pulse checks
Eberle B, Dick WF, Schneider T, Wisser G, Doetsch S, Tzanova I. Checking the carotid pulse check: diagnostic accuracy of first responders in patients with and without a pulse. Resuscitation. 1996; 33(2):107-116.
Germanoska B, Coady M, Ng S, Fermanis G, Miller M. The reliability of carotid ultrasound in determining the return of pulsatile flow: A pilot study. Ultrasound. 2018;26(2):118-126.
Ochoa FJ, Ramalle-Gómara E, Carpintero J., Garcıá A, Saralegui I. Competence of health professionals to check the carotid pulse. Resuscitation. 1998; 37(3):173-175.
Moule P. Checking the carotid pulse: diagnostic accuracy in students of the healthcare professions. Resuscitation. 2000; 44(3):195-201.
SchonbergerRB,LampertRJ,MandelEI,FeinleibJ,GongZ,HonidenS.Handheld Doppler to Improve Pulse Checks during Resuscitation of Putative Pulseless Electrical Activity Arrest: Anesthesiology. 2014; 120(4):1042-1045.
Badra K, Coutin A, Simard R, Pinto R, Lee JS, Chenkin J. The POCUS pulse check: A randomized controlled crossover study comparing pulse detection by palpation versus by point-of-care ultrasound. Resuscitation. 2019;139:17-23.
Simard RD, Unger AG, Betz M, Wu A, Chenkin J. The POCUS Pulse Check: A Case Series on a Novel Method for Determining the Presence of a Pulse Using Point-of-Care Ultrasound. J Emerg Med. 2019;56(6):674-679.
Zengin S, Gümüşboğa H, Sabak M, Eren ŞH, Altunbas G, Al B. Comparison of manual pulse palpation, cardiac ultrasonography and Doppler ultrasonography to check the pulse in cardiopulmonary arrest patients. Resuscitation. 2018;133:59- 64.
POCUS in cardiac arrest
Volpicelli G. Usefulness of emergency ultrasound in nontraumatic cardiac arrest. The American Journal of Emergency Medicine. 2011; 29(2):216-223.
Clattenburg EJ, Wroe P, Brown S, et al. Point-of-care ultrasound use in patients with cardiac arrest is associated prolonged cardiopulmonary resuscitation pauses: A prospective cohort study. Resuscitation. 2018; 122:65-68.
Huis in ’t Veld MA, Allison MG, Bostick DS, et al. Ultrasound use during cardiopulmonary resuscitation is associated with delays in chest compressions. Resuscitation. 2017; 119:95-98.
Wu C et al. The Predictive Value of Bedside Ultrasound to Restore Spontaneous Circulation in Patients with Pulseless Electrical Activity: A Systematic Review and Meta-Analysis. PLos one 2018.
Atkinson P, Bowra J, Milne J, et al. International Federation for Emergency Medicine Consensus Statement: Sonography in hypotension and cardiac arrest (SHoC): An international consensus on the use of point of care ultrasound for undifferentiated hypotension and during cardiac arrest – CORRIGENDUM. CJEM. 2017;19(4):327.
Gaspari R et al. Emergency Department Point-Of-Care Ultrasound in Out-Of-Hospital and in-ED Cardiac Arrest. Resuscitation 2016; 109: 33 – 39.
PEA arrest, arterial lines, End tidal CO2
Weingart, S. EMCrit 257 – Pulseless Electrical Activity (PEA) is Stupid. EMCrit Blog. Published on October 9, 2019. Accessed on October 22nd 2019. Available at [https://emcrit.org/emcrit/pea-is-stupid/ ]
Evidence debunking the narrow vs wide complex apch to PEA arrest by Rory Speigel on EMCrit
Kleinman ME, Goldberger ZD, Rea T, et al. 2017 American Heart Association Focused Update on Adult Basic Life Support and Cardiopulmonary Resuscitation Quality: An Update to the American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2018; 137(1):e7-e13.
Prosen G, Križmarić M, Završnik J, Grmec S. Impact of modified treatment in echocardiographically confirmed pseudo-pulseless electrical activity in out-of-hospital cardiac arrest patients with constant end-tidal carbon dioxide pressure during compression pauses. J Int Med Res. 2010;38(4):1458-67.
Littmann et al. A Simplified and Structured Teaching Tool for the Evaluation and management of Pulseless Electrical Activity. Med Princ Pract 2014. PMID: 23949188
Paradis NA, Martin GB, Goetting MG, Rivers EP, Feingold M, Nowak RM. Aortic pressure during human cardiac arrest. Identification of pseudo-electromechanical dissociation. Chest. 1992;101(1):123-8
Bergum D et al. ECG Patterns in Early Pulseless Electrical Activity- Associations with Aetiology and Survival of In-Hospital Cardiac Arrest. Resuscitation 2016. PMID: 27143124
Pierpont GL, Kruse JA, Nelson DH. Intra-arterial monitoring during cardiopulmonary resuscitation. Cathet Cardiovasc Diagn. 1985;11(5):513-20.
Venkatesh B, Clutton-brock TH, Hendry SP. Continuous intra-arterial blood gas monitoring during cardiopulmonary resuscitation. Resuscitation. 1995;29(2):135-8.
Epinephrine in cardiac arrest
Olasveengen TM, Sunde K, Brunborg C, et al. Intravenous Drug Administration During Out-of-Hospital Cardiac Arrest: A Randomized Trial. JAMA 2009;302:2222-9. 10.1001/jama.2009.1729
Olasveengen TM, Wik L, Sunde K, et al. Outcome when adrenaline (epinephrine) was actually given vs. not given – post hoc analysis of a randomized clinical trial. Resuscitation 2012;83:327-32. 10.1016/j.resuscitation.2011.11.011
Hagihara A, Hasegawa M, Abe T, et al. Prehospital Epinephrine Use and Survival Among Patients With Out-of-Hospital Cardiac Arrest. JAMA 2012;307:1161-8. 10.1001/jama.2012.294
Dumas F, Bougouin W, Geri G, et al. Is Epinephrine During Cardiac Arrest Associated With Worse Outcomes in Resuscitated Patients? J Am Coll Cardiol 2014;64:2360-7. 10.1016/j.jacc.2014.09.036
Lin S, Callaway CW, Shah, Prakesh S, et al. Adrenaline for out-of-hospital cardiac arrest resuscitation: A systematic review and meta-analysis of randomized controlled trials. Resuscitation 2014;85:732-40. 10.1016/j.resuscitation.2014.03.008
Perkins GD, Ji C, Deakin CD, et al. A Randomized Trial of Epinephrine in Out-of-Hospital Cardiac Arrest. N Engl J Med 2018;379:711-21. 10.1056/NEJMoa1806842
Loomba RS, Nijhawan K, Aggarwal S, et al. Increased return of spontaneous circulation at the expense of neurologic outcomes: Is prehospital epinephrine for out-of-hospital cardiac arrest really worth it? J Crit Care. 2015;30(6):1376–1381.
Paradis, N, Coronary Perfusion Pressure and the Return of Spontaneous Circulation in Human Cardiopulmonary Resuscitation. JAMA. American Medical Association (AMA), 1990; February 23.
Weingart, S. EMCrit Podcast 130 – Hemodynamic-Directed Dosing of Epinephrine for Cardiac Arrest. EMCrit Blog. Published on August 10, 2014. Available at [https://emcrit.org/podcasts/hemodynamic-directed-dosing-epinephrine/
Other FOAMed Resources on PEA and PseudoPEA
Rory Speigel debunks QRS width approach to PEA arrest underlying causes
Weingart – Pulseless Electrical Activity is Stupid
REBELEM on QRS width approach to PEA
EM Cases Journal Jam 14 Epinephrine in Cardiac Arrest
REBELEM on Impact of POCUS on Cardiac Arrest
EM Cases Beyond ACLS Cardiac Arrest Care with Weingart Live from EMU
CoreEM on Role of POCUS in Cardiac Arrest Care
First10EM on QRS Width Approach to PEA Arrest
Dr. Helman, Simard and Weingart have no conflicts of interest to declare
Now test your knowledge with a quiz.





Great Pod cast. Have to go back to the evidence and review my practice.
hi guys.
one of the finest pods i have ever heard.
a very fine, clear, concise, detailed discussion of this sometimes painful topic.
one of the worst cases i have had was just this.
chest pain. family drove patient (65 y.old) to the ER. arrested in the parking lot.
VF, shocked to “PEA”. stat bedside echo: stunned heart, but decent contractions on my echo. no palpable pulse.
and i had just heard a pod somewhere about the possible deleterious effects of CPR compressions on a beating heart.
i didn’t know then what i know now. and i know even more after this extraordinary pod.
It’s funny , because joe bellezzo was less gentile than scott in his characterization of “PEA” (see edecmo.org pod #13, (“PEA is bullshit”)), which is unusual.
it seems this whole topic , the biologic event, of PEA is both simple, and complicated. there is the potential for grave error both pre-hospital and in the ED., and a variety of tools to quickly discern what to do, how to proceed, and , as shown in the pod, a few variances in intelligently approaching the same problem.
incredible pod, guys. thank you Anton, Scott and Rob.
tom fiero
Which kit are folks using for femoral Arterial lines? The arrow kits seem a bit unwieldy, especially in fluffier groins. We used pediatric IJ kits often in training but not sure how ideal that is.
Also does catheter length matter in A lines? In my mind, It would make sense that longer catheter means a dampened waveform. But you’re also more central. And I’ve never heard of having to calibrate for catheter length. Be it an arrow kit or Reboa catheter. Thoughts ?
This is an amazing Podcast. Very clear. I like the pragmatic approaches to the different situations in PEA.
Thanks for your great work.