In anticipation of EM Cases Episode 110 Airway Pitfalls Live from EMU 2018 with Scott Weingart, we have Dr. Shira Brown tell her Best Case Ever of a pediatric trauma patient who required a cricothyrotomy. She explains how, despite working in a non-trauma center with limited resources, her team was well prepared because of the robust simulation program specifically designed for practicing emergency physicians that she had developed in her region. We also discuss the advantages and disadvantages of the scalpel-Bougie vs scalpel-finger-Bougie cricothyrotomy techniques and to maintain an optimistic attitude in seemingly futile cases…
Podcast Production and Sound Design by Anton Helman, May 2018
Surgical cricothyrotomy is indicated in “can’t intubate, can’t oxygenate scenarios”. This typically occurs after 3 failed DL and/or VL attempts followed by a failure to oxygenate adequately using a supraglottic device.
The procedure itself is not difficult. What is difficult (if you don’t prepare adequately) is the mental leap required to start doing the procedure. This psychological barrier can be overcome more easily if you prepare as outlined below.
The Difficult Airway Society guidelines recommend the scalpel-bougie technique.
Elements required to maximize your chances of a successful cricothyrotomy
Phase 1: Before you start your ED shift
- Familiarize yourself with a standardized challenging airway cart containing simple Bougie-assisted cric kit (Bougie, #10 scalpel, 6.0mm ETT – see image).
- Establish a cohesive “difficult airway” program in your hospital based on current guidelines adapted to your specific environment.
- Two step simulation training: low fidelity deliberate practice with simulation model (see examples SOCMOB video below and at ALiEM), followed by case-based simulation to augment psychological skills in a stressful situation.
- Post a standardized algorithm on the wall of your ED resuscitation room.
Phase 2: Before you perform the cric
- Mark the cricothyroid membrane with an indelible marker before any intubation attempt in anticipated challenging airway scenarios. This provides you and your team confidence in starting the procedure if it becomes necessary. Consider POCUS to aid in locating the cricothyroid membrane.
- Verbalize a failed airway plan and assign roles to your team.
- Clearly announce a “can’t intubate, can’t ventilate” situation.
Phase 3: The Bougie-assisted cricothyrotomy technique
- Extend the patient’s neck (unless c-spine precautions).
- Use a “laryngeal handshake” to stabilize the larynx.
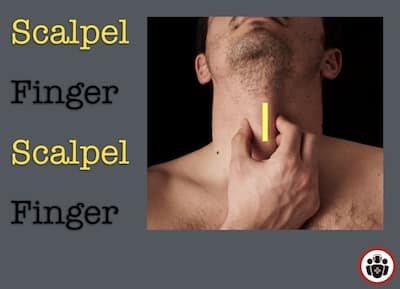
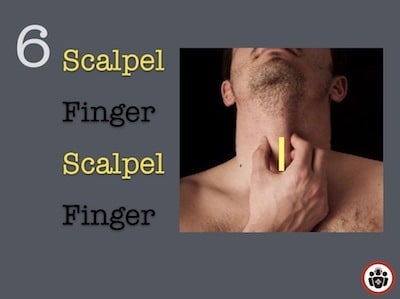
- Use the “scalpel-finger-scalpel-finger” technique (see below)
- Railroad the 6.0mm ETT over the Bougie
- Attach BVM, check tube placement and confirm end tidal CO2

Simplified Bougie-assisted Cric kit
Build your own bleeding cric simulation model at ALiEM
Scalpel-Finger-Scalpel-Finger Bougie Assisted Cricothyrotomy
After extending the patient’s neck and stablizing the larnx with a “larnygeal handshake”…
- If the cricothyroid membrane was identified prior to airway management, make a 3cm vertical incision with a #10 scalpel that crosses the cricothyroid membane. If you did not identify the cricothyroid membrane in advance of airway management make a larger incision down to the sternal notch.
- Palpate the cricothyroid membrane with your index finger.
- Make a horizontal incision with the scalpel in the cricothyroid membrane, rotate the scalpel blade 90 degrees caudally, then remove the scalpel.
- Place your index finger in the hole followed by the Bougie and the railroaded 6.0mm ETT
About Laura Duggan’s wearable cricothyrotomy trainer
Low fidelity Cric Trainer
With Chris Bond
Simulation of failed airway followed by Bougie-assisted cricothyrotomy
With Andrew Petrosoniak and Chris Hicks
Real patient Bougie-assisted Cricothyrotomy Procedure
Detailed anatomy on how to identify the cricothyroid membrane by Andy Neill
References
Frerk C, Mitchell VS, McNarry AF. Difficult Airway Society 2015 guidelines for management of unanticipated difficult intubation in adults. British journal of anaesthesia. 2015; 115(6):827-48.
Petrosoniak A, Ryzynski A, Lebovic G, Woolfrey K. Cricothyroidotomy In Situ Simulation Curriculum (CRIC Study): Training Residents for Rare Procedures. Simul Healthc. 2017;12(2):76-82.
Pracy JP, Brennan L, Cook TM. Surgical intervention during a Can’t intubate Can’t Oxygenate (CICO) Event: Emergency Front-of-neck Airway (FONA)? British journal of anaesthesia. 2016.
Kristensen, M S, W H Teoh, S S Rudolph, M F Tvede, R Hesselfeldt, J Børglum, T Lohse, and L N Hansen. 2015. Structured approach to ultrasound-guided identification of the cricothyroid membrane: a randomized comparison with the palpation method in the morbidly obese. British journal of anaesthesia, no. 6.
Scott Weingart. EMCrit Podcast 131 – Cricothyrotomy – Cut to Air: Emergency Surgical Airway. EMCrit Blog. Published on August 26, 2014. Available at [https://emcrit.org/emcrit/surgical-airway/ ].
Other FOAMed Resources on Cricothyrotomy
Justin Morgenstern’s airway series on First10EM
Bougie-aided cric by Darren Braude on EMCrit
Richard Levitan’s ACEP Now article on cric tips and tricks




Leave A Comment