In Part 1 of this Episode on Pediatric Abdominal Pain, Dr. Anna Jarvis, “the mother of pediatric emergency medicine” & Dr. Stephen Freedman, one of the world’s pre-eminent pediatric emergency medicine researchers, discuss the nuances of the history, physical and work up of Pediatric Abdominal Pain & Appendicitis and key pearls on how to distinguish serious surgical causes from the very common diagnosis of gastroenteritis. An in-depth discussion on the pearls of the history, physical exam, lab tests, imaging including serial ultrasounds vs plain CT vs CT abdomen with contrast, clinical decision rules such as the Alvarado Score, best analgesics and antibiotics in pediatric appendicitis follows.
Dr. Jarivs and Dr. Freedman answer such questions as: What is the value of a urinalysis in kids with abdominal pain? What is the next step in the work-up of pediatric appendicitis when an ultrasound is ‘equivocal’? How can we optimize the accuracy of ultrasound in kids? Should we be using contrast when ordering a CT to rule out appendicitis? What is the value of inflammatory markers in the work-up of appendicitis? Which kids with appendicitis require antibiotics in the ED? Which kids with appendicitis do not require surgery? What are the most useful tips and tricks to use during your history and physical exam to maximize your diagnostic yield? and many many more……
Podcast: Play in new window | Download (Duration: 1:20:32 — 64.6MB)
Subscribe: Apple Podcasts
Written Summary and blog post by Claire Heslop, edite by Anton Helman, December 2011
Cite this podcast as: Jarvis, A, Freedman, S, Helman, A. Part 1: Pediatric Abdominal Pain and Appendicitis. Emergency Medicine Cases. December, 2011. https://emergencymedicinecases.com/episode-19-part-1-pediatric-abdominal-pain-appendicitis/. Accessed [date].
Go to part 2 of this 2-part podcast on pediatric abdominal pain
Most Common Diagnoses for Pediatric Abdominal Pain in the ED
- In order of prevalence
- 1. Gastroenteritis
- 2. Respiratory Tract Infection (including Otitis Media, Pharyngitis and pneumonia)
- 3. UTI
- 4. Constipation
- 5. Appendicitis
- Aside from gastroenteritis, upper respiratory tract infection is the most common diagnosis written at the bottom of the emergency chart for missed appendicitis in kids!
Pediatric Appendicitis Presentation
- The majority of cases of appendicitis in children <4y/o are perorated appendicitis, probably due to the atypical presentation and delay in diagnosis in this age group
- This delay in diagnosis is due to the absence of the classic history of anorexia and vague periumbilical pain followed by migration of pain to the right lower quadrant and onset of fever and vomiting in many children
- ‘Atypical is typical’ – diarrhea, constipation and dysuria are not uncommon and may lead the clinician astray; pain may localize to the back or psoas muscle as many children have a retrocecal appendix; vomiting may occur before abdominal pain (in contradistinction to the classic abdominal pain before vomiting in appendicitis) as younger children are unable to communicate their pain
- Clues to perforation: Diarrhea is more likely to occur after perforation and temp is often higher; no localization of pain with peritoneal signs; if there is abscess formation you may feel a mass in the RLQ
Physical Exam of the Abdomen Pearls in Pediatric Patients
- Children with appendicitis are usually lying still with the hips flexed as apposed to writhing in pain
- Examine the child in their caretaker’s lap, or lying on top of their caregiver, or with their legs wrapped around their caregiver’s trunk, first with their clothes still on
- Roll the patient’s hips and look for discomfort/pain with this maneuver Have the child palpate their own abdomen
Percuss before you palpate!
- Ask the child to ‘blow out the candles’ and look for respiratory splinting as the diaphragm lowers
- The equivalent of ‘jump tenderness’ in infants and toddlers is having the caregiver bounce the child on their knee and observing for irritability
- Examine the genitals of all boys with abdominal pain to look for testicular torsion!
Value of Lab Tests in Pediatric Patients with Abdominal Pain
- About 1/4 of children with gastro will have elevated WBC (because dehydration and acidosis elevate the WBC) and many children with appendicitis will have a normal WBC; however, if the appendix is perforated, the vast majority of children will have an elevated WBC count.
Clinical Pearl:
The earlier the presentation the less likely the WBC will be elevated.
The WBC is normal in first 24hrs in 80% of appendicitis cases.
- CRP may be more sensitive than WBC in identifying a perforated appendix but cannot rule out appendicitis
- Urinalysis (clean catch or catheter specimen): useful to rule out DKA, UTI, and pregnancy in teenagers as a cause for abdominal pain; sterile pyuria is consistent with appendicitis and gastro
- ‘Finger‐prick’ Glucose: hypoglycaemia in severe gastro, hyperglycemia in DKA
Clinical Pearl:
Pyuria and hematuria are findings that can be consistent with the
diagnosis of appendicitis. Don’t let the findings of pyuria or hematuria
dissuade you from diagnosing appendicitis in a child who you suspect
has appendicitis clinically.
Imaging for Pediatric Appendicitis
- Wide variation of practice when it comes to whether or not, and how to best image children suspected of having appendicitis
- First line is ultrasound which has a very high sensitivity and specificity for appendicitis, >95% respectively, but depends on technician skill, radiologist skill, patient co‐operation, patient girth (it is more difficult to obtain good images in obese patients), and whether or not the patient is given adequate anxiolysis and analgesic
- Ultrasound criteria for appendicitis: tender and non‐compressible >6mm appendix, hyperemic appendix, wall thickness >1.7mm, plus secondary signs of thickening of mesenteric fat, free fluid, increased echogenicity, enlarged lymph nodes, abscess
- Even if the appendix is not visualized on ultrasound, appendicitis can be excluded more confidently in the patient with low clinical pre‐test probability if ultrasonography shows no secondary signs of appendicitis (eg, hyperechoic mesenteric fat, fluid collection, localized dilated small bowel loop)
If ultrasound is equivocal (eg: ‘appendix not seen’) and you still have clinical suspicion, consider surgical consultation and/or repeat physical exams, repeat blood work and repeat ultrasound
- In some centres second line imaging is repeat ultrasound (ie a repeat ultrasound in 12hrs improves accuracy)
- In other centres second line imaging is abdominal CT, which carries a life‐time cancer risk of about 1 in 1000 in children (the younger the child, the higher the risk)
- For children with a very high clinical pre‐test probability for appendicitis, consider consulting surgeon for direct appendectomy without imaging
- Some centres such as the British Columbia Children’s Hospital have a higher negative appendectomy rate for patients who do not get any imaging and go directly to the operating room and a higher perforation rate in patients who get imaging due to the delay in time to surgery
- There is likely a happy medium between imaging all patients and taking all patients directly to the operating room
Update 2023: A Canadian prospective cohort study of 624 pediatric patients (aged 4-17) with suspected appendicitis found that an US-MRI pathway where those who had a non-diagnostic ultrasound and persistent appendicitis concern or conclusive US-reassessment discrepancies underwent ultra-rapid MRI was 100% sensitive, 98.2% specific, PPV 90.5%, NPV 100%, with MRI imaging accuracy of 96.4%. The overall algorithm was found to be 98.7% accurate. Abstract
Clinical Pearl:
While the accuracy of ultrasound for the diagnosis of appendicitis increases
with time from onset of symptoms, the accuracy of CT does not change with
time. It is therefore reasonable to repeat an abdominal ultrasound in 12-24
hours for patients with a low or moderate probability of appendicitis with
an equivocal initial ultrasound, who present early after symptom onset.
For more on ultrasound vs CT for appendicitis on ALiEM go here
Pediatric Pain Management and Anxiolytics
- There is good evidence from at least 4 studies that administration of appropriate analgesics does change clinical decision‐making for appendicitis and may help the ultrasound technicians obtain a more accurate scan
- There is good evidence that children are generally undertreated for pain in the ED
- Anxiolytic medication (eg: intranasal midazolam) is helpful prior to imaging in selected patients
- Analgesics
- Morphine 0.1mg/kg (max 5mg), Fentanyl 1‐2micrograms/kg, Ketorolac 0.5‐1mg/kg
Codeine: the clinical benefit is unpredictable as there is genetic variation in its metabolism so it has been removed from some pediatric emergency department formularies
- Morphine 0.1mg/kg (max 5mg), Fentanyl 1‐2micrograms/kg, Ketorolac 0.5‐1mg/kg
Decision Rules for Pediatric Appendicitis
- There is evidence that pediatric appendicitis decision rules decrease the use of CT scans by about 20%
- Sensitivities are poor for decision rules when prospectively validated (Ann Emerg Med. 2007;49:778-784)
but may be helpful in guiding clinicians who do not see pediatric patients on a regular basis
- Alvarado Score
- >6: sensitivity = 72% (1 pt each for ‐ migration of pain to RLQ, anorexia, nausea/vomiting, tenderness in RLQ, rebound pain, fever, leukocytosis, left shift)
- Samuel Score
- (‘Pediatric Appendicitis Score’) >5: sensitivity = 82% (1pt each for – RLQ tenderness elicited by cough, hopping or percussion, anorexia, fever, nausea/vomiting, tenderness over the right iliac fossa, leucocytosis, left shit, migration of pain
Update 2019: A validation study for a pediatric appendicitis risk calculator (pARC) involving 2089 patients aged 5 years and older, showed accurate assessment of appendicitis risk in community EDs. Abstract
For more on appendicitis decision rules visit emDocs here
Treatment of Pediatric Appendicitis
- Any child with sepsis, peritonitis, perforated appendix, abscessed appendix requires broad spectrum antibiotics in the emergency department as soon as possible
- In patients with non‐perforated appendicitis, antibiotics are given pre‐operatively on call to the operating room to decrease the incidence of wound infection and abscess formation
- Patients with perforated appendicitis are usually managed conservatively with antibiotics, percutaneous drainage and interval surgery (surgery after 8‐12wks)
Update 2017: Two different meta-analyses have been published in March 2017 regarding Non-Operative Treatment (NOT) for pediatric Acute Uncomplicated Appendicitis (AUA). A meta-analysis of 5 studies (N=404) in JAMA Pediatrics found antibiotics for AUA had a success rate of 90.5%, with higher treatment failure in children with an appendicolith. A separate meta-analysis (10 studies, N=413) in Pediatrics found an initial treatment rate of 97% but a recurrence of 14% in those treated non-operatively. Overall, NOT may be an option for pediatric appendicitis but further studies need to be done prior to a change in current clinical practice. Appendectomy remains the treatment of choice at this time. Abstract 1 Abstract 2
Dr. Jarvis, Dr. Helman and Dr. Freedman have no conflicts of interest to declare.
Key References
1. Becker T, Kharbanda A, Bachur R. Atypical clinical features of pediatric appendicitis. Acad Emerg
Med. 2007; 14 (2): 124-9.
2. Bundy DG, Byerley JS, Liles EA, Perrin EM, Katnelson J, Rice HE. Does this child have appendicitis.
JAMA. 2007; 298 (4): 438-51.
3. Kharbanda AB, Casme Y, Liu K, Spitalnik SL, Dayan PS. Discriminative accuracy of novel and
traditional biomarkers in children with suspected appendicitis adjusted for duration of abdominal
pain. Acad Emerg Med. 2011; 18(6): 567-74.
4. Kwan KY, Nager AL. Diagnosing pediatric appendicitis: usefulness of laboratory markers. Am J
Emerg Med. 2010; 28 (9): 1000-15.
5. Kharbanda AB, Dudley NC, Bujaj L et al. Validation and refinement of a prediction rule to identify
children at low risk for acute appendicitis. Arch Pediatr Adolesc Med. 2012; 166 (8): 738-44.
6. Kulik DM, Uleryk EM, Maguire JL. Does this child have appendicitis? A systematic review of clinical
prediction rules for children with acute abdominal pain. Journal of Clinical Epidemiology. 2013; 66:
95-104.
7. Goldman RD, Crum D, Bromberg R, Rogovik A, Langer JC. Analgesia administration for acute
abdominal pain in the pediatric emergency department. Pediatric Emergency Care. 2006; 22 (1):
19-21.
8. Estey A, Poonai N, Lim R. Apprendix not seen: the predictive value of secondary inflammatory
sonographic signs. Pediatric emergency Care. 2006; 29 (4): 435 – 439.
9. Bachur RG, Dayan PS, Bajaj L et al. The effect of abdominal pain duration on the accuracy of
diagnostic imaging for pediatric appendicitis. Annals of Emergency Medicine. 2012; 60 (5): 582-
590.
10. Ohle R, O’Reilly F, O’Brien KK, et al. The Alvarado score for predicting acute appendicitis: a
systematic review. BMC Med. 2011;9:139.
11. Doria AS, Moineddin R, Kellenberger CJ, Epelman M et al. US or CT for diagnosis of appendicitis in
children and adults? A meta-analysis. Radiology. 2006; 241 (1): 81-94.
12. Antibiotics and appendicitis in the pediatric population: an American Pediatric Surgical
Association Outcomes and Clinical Trials Committee Systematic Review. Journal of Pediatric
Surgery, 2010, 45, 2181-2185.W
For more on pediatric abdominal pain on EM cases:
Episode 19 Part 2: Pediatric Gastroenteritis, Constipation and Bowel Obstruction
For more Pediatric EM learning visit trekk.ca – Translating Emergency Knowledge for Kids (TREKK) is a growing network of researchers, clinicians, health consumers and national organizations who want to accelerate the speed at which the latest knowledge in children’s emergency care is put into practice in general EDs – rural, remote or urban.

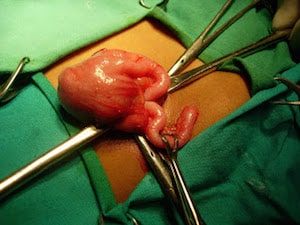




Patients with perforated appendicitis are usually managed conservatively with antibiotics, percutaneous drainage and interval surgery (surgery after 8‐12wks). ???????
I am a surgeon,and this is complete nonsense!!
Thanks for your comment. At the time of this podcast this was the recommended management for perforated appendicitis (http://emedicine.medscape.com/article/773895-treatment#d12). Subsequently there have been studies such as (Bonadio W, Rebillot K, Ukwuoma O, Saracino C, Iskhakov A. Management of pediatric perforated appendicitis: comparing outcomes using early appendectomy vs solely medical management. Pediatr Infect Dis J. 2015 Dec 14. [Medline].) that have suggested that early surgery may be superior.