In this Part 2 of EM Cases’ Highlights from Whistler’s Update in EM Conference 2015 Dr. David Carr gives you his top 5 pearls and pitfalls on ED antibiotic use including when patients with sinusitis really require antibiotics, when oral antibiotics can replace IV antibiotics, how we should be dosing Vancomycin in the ED, the newest antibiotic regimens for gonorrhea and the mortality benefit associated with antibiotic use in patients with upper GI bleeds. Dr. Chris Hicks gives you his take on immediate PCI in post-cardiac arrest patients with a presumed cardiac cause and The Modified HEART Score to safely discharge patients with low risk chest pain.
Written summary & blog postPrepared by Dr. Keerat Grewal & Dr. Anton Helman, May 2015
Cite this podcast as: Helman, A, Carr, D, Hicks, C. Highlights from Whistler’s Update in EM Conference 2015 Part 2. Emergency Medicine Cases. May, 2015. https://emergencymedicinecases.com/highlights-whistlers-update-in-em-conference-2015-part-2/. Accessed [date].
5 Antibiotic Pearls and Pitfalls
1. Sinusitis & Pharyngitis rarely require antibiotics
How to identify acute bacterial vs viral sinusitis
From IDSA Guidelines (2012)
1 of 3 presentations make bacterial sinusitis more likely:
- Onset with persistent symptoms or signs compatible with acute rhinosinusitis with symptoms lasting 10 or more days, without any evidence of improvement
- Onset with severe symptoms or signs of high fever (>39.0 C), purulent nasal discharge, or facial pain lasting at least 3-4 consecutive days at the beginning of illness
- Onset with worsening symptoms or signs characterized by the new onset of fever, headache or increase in nasal discharge following a typical URI that lasted 5-6 days that were initially improving.
Dr. Carr recommends treating sinusitis with antibiotics only in immunocompromised patients, post-op patients and septic patients, as most are viral and the NNT to shorten the duration of illness is 13.
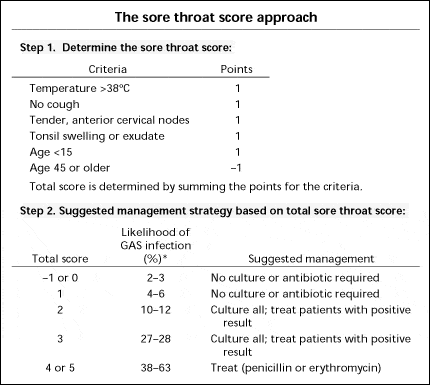
McIassac Pharyngitis Score
Dr. Carr’s Commentary: Antibiotics are rarely (if ever) required for pharyngitis in adults as most cases are viral, only approximately 50% of patients with a McIssac score of 4 or 5 have strep throat, rheumatic fever in adults is extremely rare in North America (with little evidence that antibiotics prevent it), and the NNT to prevent suppurative complications of strep throat is approximately 400.
Oral Penicillin for Pharyngitis: Number Needed to Harm
NNH = 5000 for anaphylaxis
NNH = 10 for diarrhea
*Note that there are still cases of pediatric rheumatic fever in Canada, and so withholding antibiotics for children with strep throat is not recommended at present.
2. Consider the bioavailability of oral antibiotics before you pull the trigger and give IV antibiotics
High Bioavailability oral antibiotics to consider instead of IV antibiotics:
Cephalexin
Quinolones – eg. ciprofloxacin, levofloxacin
Trimethoprim-Sulphamazoxazole – eg. Septra, bactrim
Clindamycin
Metronidazole
Doxycycline
Linezolid
3. Approriate Vancomycin Dosing
Use weight-based dosing of vancomycin (20-30 mg/kg based on severity of illness) rather than simply 1g or 2g. This will prevent the historical under-dosing vancomycin.
4. New Antibiotic choices for Gonorrhea
From 2014 Toronto Public Health
Uncomplicated gonorrhea: azithromycin + ceftriaxone regardless of whether the patient is positive for chlamydia.
PID: ceftriaxone + doxy +/- azithromycin 2g qweekly x2
Consider single dose gentamycin or gemifloxacin + azithromycin in high risk populations (i.e. men who have sex with men)
See The Skeptics Guide to EM for analysis of this study
5. Antibiotics for Upper GI Bleeds in cirrhotic patients
A Cochrane review meta-analysis in 2011 showed an all-cause mortality benefit in using prophylactic antibiotics in cirrhotic patients with upper GI bleeds.
Consider IV ceftriaxone for ED patients with upper GI bleeds.
Immediate PCI in all Post-Cardiac Arrest Patients with a presumed cardiac cause
PROCAT – Parisian Region Out of Hospital Cardiac Arrest Registry:
- 714 out of hospital cardiac arrest
- Excluded patients with obvious non-cardiac cause
- 400 patients underwent immediate angiography +/- PCI.
- Findings: ECGs that had ST elevations were specific (96%) for coronary lesions requiring PCI, however, lacked sensitivity. In patients with non-diagnostic ECGs, 60% of patients had lesions deemed appropriate for coronary stenting
A significant mortality benefit was shown for early angiography +/- PCI in post-cardiac arrest patients regardless of whether the ECG showed a STEMI or NSTEMI pattern.
AHA (2013) Recommendations:
- Immediate coronary angiography (and PCI when indicated) should be performed in resuscitated out of hospital cardiac arrest patients when the initial ECG shows STEMI.
- Despite the absence of STEMI, it is reasonable to consider immediate angiography in patients that have a non-obvious cause of the arrest and an ischemic cause is deemed most likely on clinical grounds
Dr. Hicks’ Commentary: ED physicians should advocate for their patients to go for immediate angiography +/- PCI when they have non-diagnostic ECGs and a presumed cardiac cause of their out-of-hospital cardiac arrest.
The Modified Heart Score for Low Risk Chest Pain
The original 5 point HEART Score from the Netherlands
For patients at low risk for Major Adverse Cardiac Events (MACE) in the ED setting (i.e. PCI, CABG, death).
This study used a single traditional troponin assay (not the high-sensitivity troponins that are increasingly being used) regardless of the timing of the troponin. Most EM providers would agree that a rate of MACE of 2.5% is not low enough to discharge patients from the ED. However, the Modified HEART Score lowered the risk of MACE to 0.6% by adding high sensitivity Troponins at 0 and 3 hours after arrival at the ED.
The Modified HEART Score
- HEART Score < 3, and
- Negative high sensitivity troponins at 0 and 3 hours
The rate of MACE in these patients was 0.6% within 6 weeks.
A subsequent study in March 2015 using the modified HEART score showed significant decreases in objective cardiac testing and median length of stay and increases in early discharge rates while maintaining a zero MACE rate at 30 days.
Another Approach to Low Risk Chest Pain (unpublished)
NICE (National Institute for Clinical Excellence) in the UK has suggested that negative high sensitivity troponins at 0 and 3 hours in any population, regardless of risk, may rule out ACS and patients can be discharged home for outpatient work up.
Additional FOAMed resources on the HEART Score & modified HEART score
Emergency Medicine Literature of Note
ERCast with Amal Mattu
Key References
Chow AW, Benninger MS, Brook I et al. 2012. IDSA clinical practice guidelines for acute bacterial rhinosinusitis in children and adults. Clin Inf Dis. Full PDF
Kirkcaldy et al. The efficacy and safety of Gentamicin plus Axithromycin and Gemifloxacin plus Azithromycin as treatement of uncomplicated Gonorrhea. Clinical Infectious Diseases. 2014. Full PDF
Chavez-Tapia e al. Meta-analysis: antibiotic prophylaxis for cirrhotic patients with upper gastrointestinal bleeding – an updated Cochrane review. Alimentary Pharmacology and Therapeutics. 34;509-518, 2011. Full PDF
Bangalore, S & Hochman, JS. 2010. A routine invasive strategy for out-of-hospital cardiac arrest survivors: Are we there yet? Circulation: Cardiovascular Interventions, 3: 197-9. Full PDF
Backus BE, Six AJ, Kelder JC, et al. 2013. A prospective validation of the HEART score for chest patients at the emergency department. Int J of Cardiology, 168(3): 2153-8. Abstract
Mahler SA et al. The HEART Pathway Randomized Trial Identifying Emergency Department Patients With Acute Chest Pain for Early Discharge. Circ Cardiovasc Qual Outcomes March 2015; 8 (2): 195 – 203. Abstract
Six AJ, Backus BE & Kelder JC. 2008. Chest pain in the emergency room: Value of the HEART score. Neth Heart J: 16(6): 191-6. Abstract
Dr. Helman, Dr. Carr & Dr. Hicks have no conflicts of interest to declare






Leave A Comment