When patients with known congenital heart disease present to the ED with common illnesses we need to consider how their physiology might alter our approach to those common illnesses. Max Ben-Yakov guides us through his Best Case Ever of a CHD patient who presents with bronchiolitis and gives us some tips on how best to approach these fragile patients in a crisis situation…
Podcast: Play in new window | Download (Duration: 15:57 — 14.6MB)
Subscribe: Apple Podcasts
Podcast production by Anton Helman and Max Ben-Yakov
Editing and sound design by Anton Helman February 2018
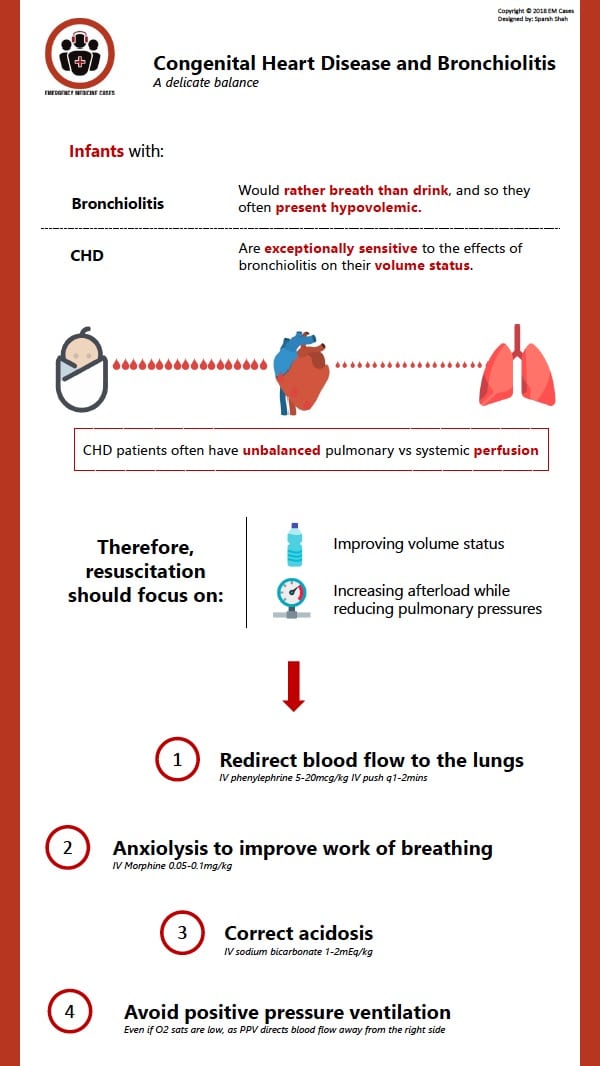
Patients with CHD are exceptionally sensitive to the effects of bronchiolitis on their volume status
While we tend to think of bronchiolitis as a purely respiratory illness, young infants with CHD are exceptionally sensitive to the effects of bronchiolitis on their volume status. Patients with bronchiolitis would rather breath than drink, and so they often present hypovolemic.
CHD patients often have unbalanced pulmonary vs systemic perfusion. In the resuscitation of these patients the focus should be on a) improving volume status b) increasing afterload while reducing pulmonary pressures.
While most children with mild gastroenteritis or bronchiolitis can be discharged from the ED safely, your threshold for admitting CHD patients with a mild viral illness should be much lower.
Four principles of treating a Tet Spell
1.Redirect blood flow to the lungs. In a Tet spell your aim is to redirect the blood from the left side of the heart to the right side of the heart to improve pulmonary blood flow by increasing afterload. You can achieve this with IV phenylephrine 5-20mcg/kg IV push q1-2 minutes (add 10mg of phenylephrine to a 1L bag of normal saline so that the concentration is 10mcg/ml).
2.Anxiolysis to improve work of breathing. Give IV morphine 0.05-0.1mg/kg.
3.Correct acidosis. Give IV sodium bicarbonate 1-2mEq/kg.
4.Avoid positive pressure ventilation when possible as it directs blood flow away from the right side of the heart where the Tet spell patient needs it most, even if the patient’s oxygen saturation is very low.
Drs Ben-Yakov and Helman have no conflicts of interest to declare.





Great case..