In anticipation of EM Cases Episode 112 on Tachydysrhthmias with Amal Mattu and Paul Dorion, Dr. Melanie Baimel tells her Best Case Ever of a previously healthy young man who presents in refractory ventricular fibrillation after receiving multiple single shocks, ongoing chest compressions, several rounds of epinephrine, amiodarone and dual sequence defibrillation without ROSC…
Podcast production, editing, sound design and summary by Anton Helman, July 2018
Infographic by Sparsh Shah
Why esmolol for refractory Ventricular Fibrillation?
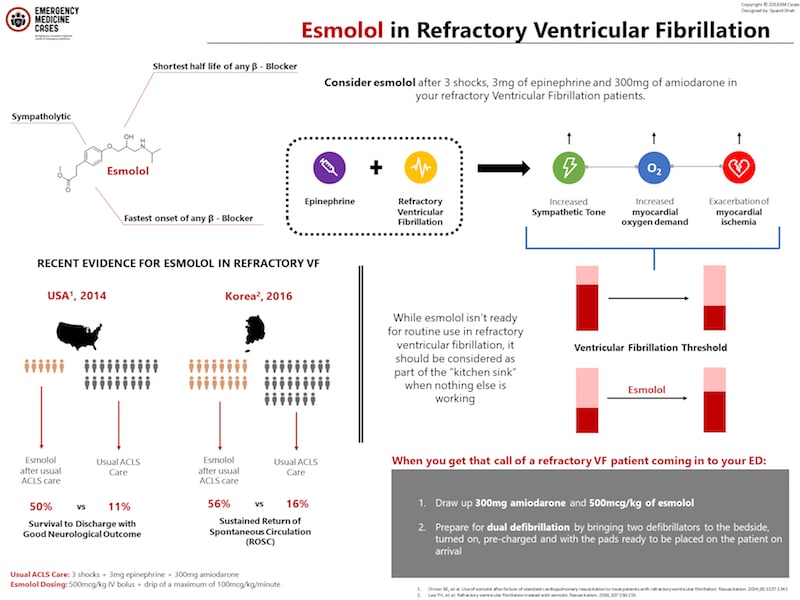
In refractory Ventricular Fibrillation there is a huge increase in sympathetic tone at least partially due to the epinephrine given, which results in increased myocardial oxygen demand, exacerbation of myocardial ischemia, and depression of the VF threshold. Esmolol is the perfect sympatholytic and it increases the fibrillation threshold. It has the fastest onset and shortest half-life of any B-blocker.
What is the evidence for esmolol for refractory Ventricular Fibrillation?
The evidence for esmolol in refractory Ventricular Fibrillation isn’t the greatest – no big RCTs to be certain. There are a handful of older small studies looking at other B-blockers in cardiac arrest that looked promising, but these were done in an era of cardiac arrest management that is now considered archaic. The evidence we have for esmolol in refractory VF in particular comes from 2 more recent studies performed in the latest era of ACLS management.
A 2014 out of a single center in the U.S. compared 6 patients who got esmolol after usual ACLS care with 19 controls who just got usual ACLS care. All 6 patients achieved ROSC after 500mcg/kg IV bolus followed by a drip of a maximum of 100mcg/kg/minunte – with 4 of them achieving s
ustained ROSC. And here’s the amazing part – survival to discharge with a good neurologic outcome was 50% in the esmolol group vs 11% in the control group. Tiny study with impressive results.
Then in 2016 there was another retrospective study of out of hospital cardiac arrests in Korea comparing 16 patients who got esmolol to 25 patients who didn’t. They used the same dosing of esmolol as the previous study, again after usual ACLS care – 3 shocks, 3mg of epinephrine and 300mg amiodarone – and they found similar outcomes: improved rates of ROSC and survival to the ICU.
So while we’re waiting for some bigger multicentre RCTs, for now, consider esmolol after 3 shocks, 3mg of epi and 300mg of amiodarone in your refractory Ventrcular Fibrillation patients. While esmolol isn’t ready for routine use in this setting, it should be considered as part of the “kitchen sink” when nothing else is working.
Logistics of using esmolol for refractory Ventricular Fibrillation
When you get that call patched in of a refractory VF patient coming in to your ED, premix 300mg of amiodorane, 500micrograms/kg of esmolol and prepare for dual defibrillation by bringing two defibrillators to the bedside, turned on, pre-charged and with the pads ready to be placed on the patient on arrival.
If all that doesn’t work there’s always the old ultrasound guided stellate ganglion block that will take out sympathetic drive to the heart – I know, sounds like kind of a crazy move – but again, you ain’t got nothin’ to lose.
References
Driver BE, Debaty G, Plummer DW, Smith SW. Use of esmolol after failure of standard cardiopulmonary resuscitation to treat patients with refractory ventricular fibrillation. Resuscitation. 2014;85:1337-1341.
Lee YH, et al. Refractory ventricular fibrillation treated with esmolol. Resuscitation. 2016;107:150-155.
de Oliveira FC, Feitosa-Filho GS, Ritt LE. Use of beta-blockers for the treatment of cardiac arrest due to ventricular fibrillation/pulseless ventricular tachycardia: a systematic review. Resuscitation. 2012;83:674-83.
Meng L, Tseng CH, Shivkumar K, Ajijola O. Efficacy of Stellate Ganglion Blockade in Managing Electrical Storm: A Systematic Review. JACC Clin Electrophysiol. 2017;3(9):942-949.
Other FOAMed Resources on Esmolol for Refractory Ventricular Fibrillation
EM Cases Episode 96 Beyond ACLS Cardiac Arrest Live from EMU 2017





If the goal is to reduce sympathetic drive, why are we still “jacking people up” with epinephrine first? Last I checked there remained no affirmative evidence that it leads to increased rates of hospital discharge and a large Japanese study that actually showed harm from Epi use?
Why increase a frenetic drive with epinephrine if the goal is to cool off adrenergic drive with esmolol. Little or no evidence to support ROSC to hospital d/c with epi use?
Adrenergic…. not frenetic