There is something indescribable that happens when the overhead speaker crackles overhead with “Code Pink”. The stakes are high, and every person in the building collectively holds their breath. It’s in the air. All the more reason to know neonatal resuscitation better than the back of your hand. This is not an easy task. We’re talking about – hopefully – once-in-a-career events that require expertise, precision, and outstanding team dynamics. Resuscitation of the sick newborn is a HALO situation – High Acuity Low Opportunity for most of us. But there are few things in medicine more worthwhile knowing. Now, just to get things in perspective, thankfully about 90% of births are uncomplicated requiring just a quick overall assessment, a clamp and cut of the cord and placing the baby on mom’s chest to keep them warm. Of the remaining 10% – almost all of them just require just a bit of help – some stimulation and a bit of oxygen – easy stuff. But, of the births we manage in the ED a small percentage will require advanced resuscitation. Dr. Hilary Whyte, Dr. Jabeen Fayyaz and Dr. Emily MacNeil guide us through the AHA neonatal resuscitation algorithm box by box and highlight key strategies, techniques and equipment, and also some major pitfalls in early resuscitation…
Podcast production, sound design & editing by Anton Helman
Written Summary and blog post by Lorraine Lau & Winny Li, edited by Anton Helman May, 2020
Infographic by Sarah Foohey
Cite this podcast as: Helman, A. Whyte, H. Fayyaz, J. MacNeil, E. Episode 142 – Neonatal Resuscitation. Emergency Medicine Cases. May, 2020. https://emergencymedicinecases.com/neonatal-resuscitation. Accessed [date]
General approach to neonatal resuscitation
- ABC rather than CAB as recruitment of the lungs using positive pressure support, oxygenation and ventilation takes precedence over chest compressions
- Goals of resuscitation: “warm, pink and sweet”
- Prepare yourself, your team and your gear
Preparation
- Yourself: box breathing, positive self-talk, visualization, tell the mother that “we’ve got this”
- Your team: call on RT, anesthesia, pediatrics, team debrief
- Your gear: a warmer and a box of NRP equipment prepared in advance in the ED
NRP Gear
Delayed cord clamping
Consider delayed cord clamping in all vigorous neonates with good tone. Delaying clamping and cutting of the umbilical cord (60-90 seconds after birth) improves blood transfusion from the placenta to neonate with benefits such as decreasing the rate of intraventricular hemorrhage and necrotizing enterocolitis in preterm infants. While an increased rate of jaundice has been associated with delayed cord clamping, there are rarely any significant clinical sequelae.
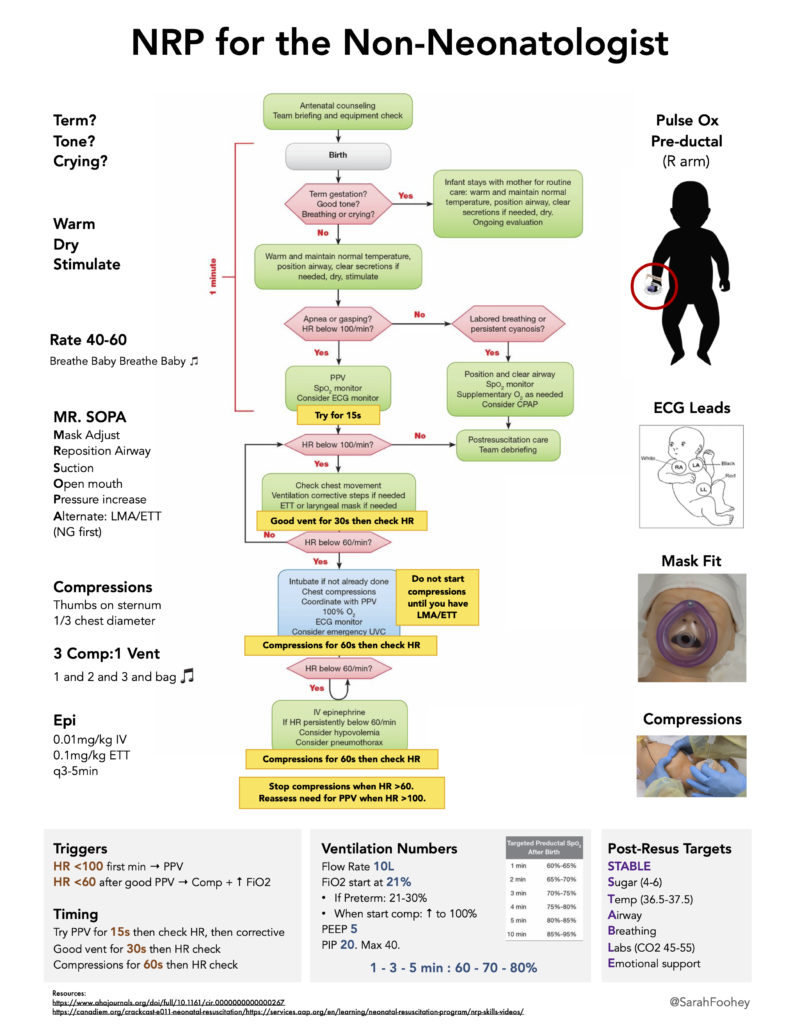
AHA Neonatal Resuscitation Algorithm
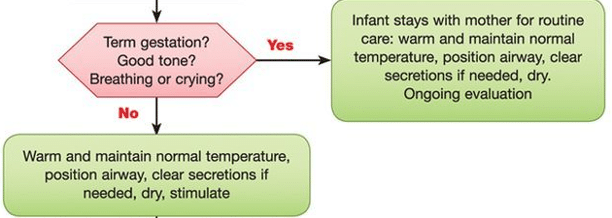
BOX 1
Term? Good tone? Breathing or crying?
If “Yes” (the neonate is term, has good tone and is breathing or crying) position airway, dry with towels, place infant on mother’s chest.
If “No” (the neonate is not term, does not have good tone or not breathing or crying) priorities are to warm the infant (see below), position the airway and stimulate.
*Routine suctioning of secretions or meconium is no longer recommend unless overt airway obstruction is present
Temperature management in the neonate: warming options and goals
Newborns lose heat rapidly. Hypothermia has been associated with increased mortality, intraventricular hemorrhage, respiratory complications, hypoglycemia dn late onset sepsis. Warm the infant who is >32 weeks gestational age with good tone and respirations by drying the neonate with a towel and placing them on their mother’s chest. Options for warming the neonate who is ≤32 weeks, has abnormal tone or respirations include:
- Place the neonate in an infant warmer set to 25˚C.
- Place the wet infant (do not dry the infant) directly in a plastic bag up to their neck
- Thermal mattress (noninferior to infant warmer)
- Heated blankets
Do not towel dry the preterm infant <32 weeks gestational age as the skin is very fragile.
Target temperature is 36.5-37.5˚C axillary
Key concept: avoid hypothermia at all costs as it is associated with increased mortality, intraventricular hemorrhage, respiratory complications, hypoglycemia and late onset sepsis.
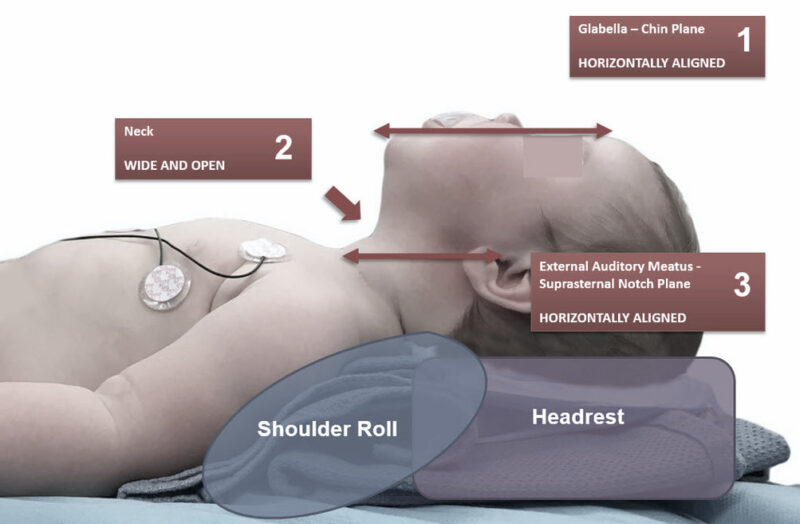
Positioning the airway on the neonate in the sniffing position
Compared to adults, neonates have larger tongues, tonsils, epiglottises and occiputs. Key positioning/airway maneuvers taking these differences into account are:
- Roll under the shoulders shifts the head to neutral/slightly extended position; may require headrest in addition to achieve the following:
- Align the chin with the glabella
- Ensure that the anterior neck space is open
- Align the external auditory meatus horizontally with the suprasternal notch
- Tongue lift: lifting the tongue with a jaw thrust and/or placement of an oral or a nasal airway is essential to minimize upper airway obstruction in a sedated or obtunded neonate.
Pitfall: Hyperextension of the head on the neck may result in airway obstruction; be sure to position the head and neck in a neutral “sniffing” position which may require a roll under the shoulder, head rest, tongue lift and jaw thrust.
Pediatric Digital Anesthesia Handbook airway positioning
Clearing secretions of the neonate
The primary focus should be on lung recruitment, oxygenation and ventilation. Previous routine nasopharyngeal and oral suctioning is no longer recommended. Even when meconium is present, suctioning is not recommended unless it is causing complete airway obstruction.
Stimulation of the neonate
Stimulate with rubbing the back or assertive flicking of the soles of the feet until the infant cries. Towel drying in the well infant >32 weeks gestational age provides stimulation as well.
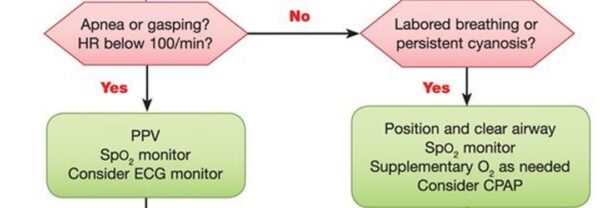
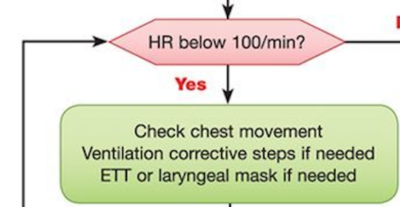
BOX 2 & 3
If the infant has labored breathing or persistent cyanosis, but HR is > 100:
- Reposition and clear airway if you haven’t already
- Jaw thrust
- Place SpO2 monitor to guide resuscitation (pre-ductal with oxygen saturation monitor on the right hand or wrist)
- Apply supplemental O2 as needed, consider positive pressure ventilation
- Heart rate monitoring with 3-lead ECG
If the neonate is apneic or gasping or has a HR <100, provide positive pressure ventilation in addition to above steps
Target 40 breaths/minute and effective ventilation.
Measuring the heart rate of the neonate: The 3-lead ECG
Obtaining an accurate heart rate measurement is of utmost importance as it helps guide resuscitation and is the most sensitive indicator of adequate resuscitation as a normal heart rate reflects adequate oxygenation/ventilation. Place an oxygenation saturation monitor on the neonate’s right hand or wrist. It is important to realize that the oxygen saturation monitor may take time to pick up and display the oxygenation saturation, that palpation of the umbilical stump is unreliable, and that auscultation is often difficult in a noisy environment. The most accurate and efficient method to measure the heart rate is using a 3 lead ECG.

3-lead ECG lead placement
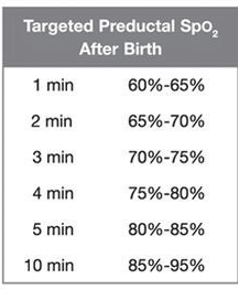
Neonatal oxygenation
Ventilation is more important than oxygenation as it takes about 10 minutes for babies to normally achieve “normal” oxygen saturation levels. Oxygen saturation targets in newborns are much lower than in adults and normally gradually rise over the first 10 minutes.
- For term and late-preterm newborns (≥35 weeks) receiving respiratory support at birth, the initial use of 21% oxygen is reasonable
- For preterm newborns (<35 weeks) receiving respiratory support at birth, it may be reasonable to begin with 21% – 30% oxygen then titrate based on pulse oximetry
- 100% FiO2 should not be used to initiate resuscitation as it is associated with increased mortality
Neonatal ventilation
Mask Ventilation
While general recommendations for sizing of oxygen masks in neonates are size 0 for preterm, round type and size 1 for term infant, use the mask that fits well over bridge of nose to chin to minimize air leak. Ensure open mouth and jaw thrust while minimizing pressure on the submental tissue to avoid tongue obstruction. Two-person technique is preferred. Avoid over ventilation while bagging by applying just enough pressure to the bag to cause adequate chest rise or PIP of 20.
Pitfall: over-bagging leading to pneumothorax and/or pneumomediastinum is not uncommon; avoid over-bagging by applying just enough pressure to the bag to cause adequate chest rise or PIP of 20.
Deliver PPV through T-piece resuscitator or flow-inflating bag, providing:
- CPAP – PEEP 5-8
- PPV – PIP 20 or until chest rise
Key concept: continuous positive airway pressures and positive end-expiratory pressures are required to open up the alveoli and to recruit the lungs
BOX 4
Corrective ventilation steps after 30 seconds of ventilation
After 30 seconds of ventilation, if no effective improvement in clinical status, remember “MR SOPA” for corrective ventilation steps
Box 5
After 30 secs of PPV, reassess HR. If HR >100 – continue PPV 40-60 breaths/min there is spontaneous effort. If HR <60, establish adequate ventilation before beginning chest compressions. Ventilation is the main priority.
Establish advanced neonatal airway within 40 seconds
The goal is to establish an advanced airway in <40 seconds, as delays beyond this are associated with increased morbidity and mortality. Strongly consider using a supraglottic airway (SGA) rather than BVM and endotracheal intubation in neonates ≥34 weeks GA and ≥1.5kg requiring advanced airway management. A Cochrane review in 2018 found that SGA demonstrated comparable efficacy to endotracheal intubation. When compared to BVM, SGA was associated with shorter resuscitation and ventilation times, and less requirement for endotracheal intubation.
Caveats for SGA
- Cannot use in infants <34 weeks or <1.5kg (no SGA small enough)
- No evidence for giving epinephrine through SGA
- Unclear if asynchronous chest compressions can be given with SGA
Key concept: You have 40 seconds to secure the airway of a sick neonate; SGA is your tool of choice in sick neonates > 34 weeks.
Pitfalls of SGA use
- If SGA is inserted too far, the esophagus can be fully intubated and distended by the SGA tip, which would require it to be withdrawn slightly.
- Bending the epiglottis over the laryngeal inlet can cause significant airway obstruction that may be resolved by repositioning of the SGA and/or the neonate’s head and neck.
- Tip of the SGA can fold on itself during insertion, preventing effective gas exchange. This can generally be corrected by withdrawing the SGA such that it is no longer folded over and then reinserting it.
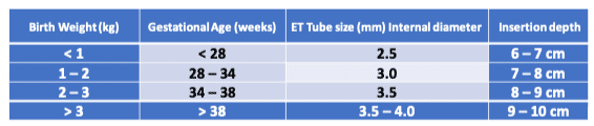
Neonatal endotracheal intubation sizing
ETT size
*have tubes half size bigger and half size smaller available
Blade size
Term infant: #1 Miller blade, 3.5mm
Preterm infant: 0 Miller, 3.0mm
ETT depth = 6 cm + weight in kg
VL or DL? Which one is preferred?
Video laryngoscopy has been associated with improved success in tracheal intubation and a decreased risk of complications in neonates compared to direct laryngoscopy.
RSI medications in neonatal resuscitation
Premedication and neuromuscular blockade use have been associated with improved intubation success and decreased complications in neonates. RSI medications have been shown to improve glottic visualization, decrease the number of intubation attempts, and decreases airway trauma.
Rule of 2s for neonatal RSI medications
Atropine 0.02 mg/kg IV
Fentanyl 2 mcg/kg IV
Succinylcholine 2 mg/kg IV
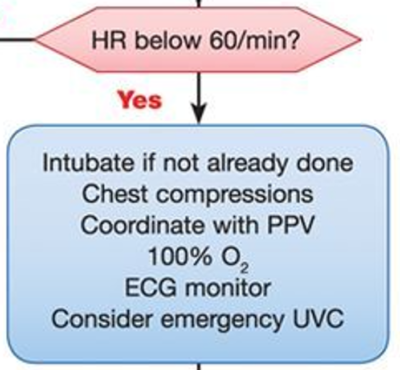
Chest compressions in neonatal resuscitation
Ensure adequate ventilation is established first. Securing an advanced airway and initiating positive pressure ventilation is strongly recommended before starting chest compressions.
Technique: 2 thumb technique on lower 1/3 of sternum to a depth of 1/3 chest diameter, ideally from head of bed is preferred over the 2 finger technique and has been shown to improve chest compression quality
Rate: 3:1 coordinated with PPV (90 compressions: 30 ventilations/min) = “1 and 2 and 3 and breathe” = 120 events per minute
Duration: 60 secs between pulse checks
Vascular Access in neonatal resuscitation: Umbilical vein catheter or IO?
Umbilical vein catheter is the preferred route. Intraosseous access is only suitable for term infants > 3kg, requiring a slightly more caudal approach than in older children, and immediate anchoring given the thinner bone cortex in neonates.
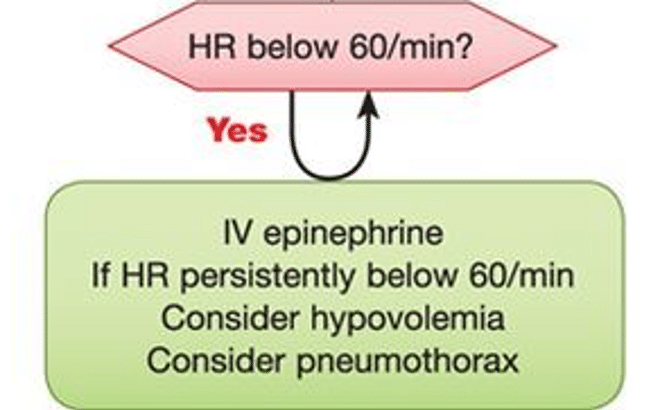
Box 6
If the HR is remains <60 after 90 seconds of effective PPV and 60 seconds of chest compressions, add epinephrine, consider hypovolemia and pneumothorax
Epinephrine dosing in neonatal resuscitation
Draw up in a 1 mL syringe and label “for IV/UVC”
0.1 mL/kg by IV
0.1 – 0.3mL (remember 0.2 in “rule of 2” for simplicity)
First dose can be given through ETT while establishing IV access.
After 120 seconds of effective PPV and 90 seconds of chest compressions, add a fluid bolus.
DOPE mnemonic in neonatal resuscitation
In scenarios where there is difficulty ventilating or oxygenating, consider the DOPE mnemonic to research for potential causes
Fluid and glucose management in neonatal resuscitation
Unlike older children and adults neonatal arrest is very rarely due to hypovolemia, so aggressive fluid resuscitation is rarely a priority in this age group.
Start with NS bolus of 10 mL/kg over 20 minutes. If a second bolus is required, consider at this time adding an inotrope.
Check the capillary glucose and provide 2 mL/kg DW10 bolus within 30 mins of birth to avoid hypoglycemia.
Goals of resuscitation
Take home points for neonatal resuscitation
- ABC rather than CAB as recruitment of the lungs using positive pressure support, oxygenation and ventilation takes precedence over chest compressions
- Goals of resuscitation: “warm, pink and sweet”
- Prepare yourself, your team and your gear and call for help early
- Avoid hypothermia at all costs using an infant warmer at 25˚C or thermal mattress, plastic bag for ≤32 wks GA or unwell, targeting axillary temperature of 36.5-37.5 ˚C
- Consider delayed cord clamping (60-90 secs) in all vigorous neonates with good tone
- Ensure optimized airway positioning in “sniffing position”
- Nasopharyngeal suctioning is reserved only for neonates with complete airway obstruction
- Drying the neonate is reserved for well appearing newborns > 32 weeks GA; all other newborns should be placed, wet, in a plastic bag up to their neck
- Place an oxygenation saturation monitor on the neonate’s right hand/wrist to measure pre-ductal saturation
- Obtain accurate heart rate measurement by 3 lead ECG
- SGA is faster and associated with better outcomes than ETT but there is no SGA that is small enough for preterm babies <34 weeks
- Ventilation is more important than oxygenation as it takes about 10 minutes for babies to normally achieve “normal” oxygen saturation levels
- Neonates are rarely hypovolemic and the initial bolus is NS bolus 10ml/kg over 20 mins
- Rule of 2s for RSI: Atropine 0.02 mg/kg IV, Fentanyl 2 mcg/kg IV and Succinylcholine 2 mg/kg IV
- Corrective ventilation steps: MR SOPA mnemonic
- Troubleshooting post intubation: DOPE mnemonic
- Targets of resuscitation: STABLE mnemonic
Additional resources:
Rural neonatal resuscitation- EM Quick Hits 38 (11:40)
Newborn resuscitation algorithm- Episode 32- Whistler Update in Emergency Medicine Conference 2013
References for neonatal resuscitation
- Escobedo MB, Aziz K, Kapadia VS, et al. 2019 American Heart Association Focused Update on Neonatal Resuscitation: An Update to the American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Pediatrics. 2020;145(1).
- Qureshi MJ, Kumar M. Laryngeal mask airway versus bag-mask ventilation or endotracheal intubation for neonatal resuscitation. Cochrane Database Syst Rev. 2018;3:CD003314.
- Soar J, Maconochie I, Wyckoff MH, et al. 2019 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations: Summary From the Basic Life Support; Advanced Life Support; Pediatric Life Support; Neonatal Life Support; Education, Implementation, and Teams; and First Aid Task Forces. Circulation. 2019;140(24):e826-e880.
- Park RS, Peyton JM, Kovatsis PG. Neonatal Airway Management. Clin Perinatol. 2019;46(4):745-763.
Drs. Helman, Whyte, Fayazz and MacNeil have no conflicts of interest to declare
Now test your knowledge with a quiz.





Do you use an oropharyngeal airway?
You may only have an ambubag with PEEP but not T piece resuscitator or flow inflating bag .or lite saver manometer .
Thanks Anton for putting this episode together, fantastic update!
anton
that was /is one the finest, most extraordinary pods i have ever listened to.
your guest speakers were succinct, expert, kind, clear and wonderful.
i’ve been an ER doc since 1986.
i work in a large busy rural community hospital with scant peds service; we ship out all sick children, admit none.
it seems whenever here is a neonate/infant or an “eye complaint” on the master board, no one is anxious to jump in and see that patient, pick up that chart.
sick children are frightening, i think.
very sick children is the substance for nightmares.
i must say that after this pod, i feel a tiny less panicked. a little better prepared. this was superb.
and yes, i too shall sign up for that course.
thank you!
(i miss you guys up north)
tom fiero, ED in merced california.
Much Appreciated NRP review and pearls!
Hi Anton, great lecture as always.
I just have a question. Can you please clarify the issue of “putting a baby in bag”. I am having a bit of trouble getting my head around it.
Do I literally put the baby in a plastic bad with the head out?
Yes! Place the baby feet first into a plastic bag while they are still wet (no drying required) with the opening of the bag at the neck.
Great talk, I presume the ETT table is uncuffed tubes? Consider specifying
Another quick down and dirty way to know ETT size for neonates is Gestational Age/10. You have to do a bit of tweaking…i.e. 27 weeks/10=2.7 which is not a tube size so go for 2.5. Then you can use the other quicks: Tube size x3=rough depth of insertion; Tube size x2=suction catheter size that will fit into ETT; Tube size x4=chest tube size.
This was an awesome podcast. Thank you for doing what you do!